
At each check-up your current medical and dental histories will be thoughtfully reviewed and updated. It is important to update current medications and allergies as well as any heart treatments, joint replacements, or any additional chronic conditions being treated by your physician. This will help us to provide you full scope treatment with the knowledge of your particular health variables. A blood pressure reading will also be taken at the beginning of appointments as a courtesy. Frequently patients are not being seen regularly by a physician and we value overall health as well as oral health.
Preventive, regular dental cleanings are an integral part of the check-up visits. Chief concerns should be brought to the attention of your hygienist upon arrival and appropriate dental x-rays will be exposed, evaluated, and discussed. We use the most advanced digital x-ray equipment to provide a safe and efficient experience for our patients. Your hygienist will remove all bacteria- harboring plaque and tartar buildup from along the gumline and between the teeth which may have been missed by brushing and flossing. This time spent also represents an important opportunity for hygiene education of home care methods that will maintain and protect your healthy smile for years to come. A final detailed polishing of the teeth will leave your mouth feeling fresh and clean long after your dental visit.
A thorough examination will be performed of your dentition and oral soft tissues as well as external supporting areas of the head and neck, including TMJ(jaw joints). These regular screenings will allow us to vigilantly monitor any development of common dental conditions such as tooth decay and gum disease and additionally less common oral symptoms which may evidence a deeper systemic issue. Externally, swollen glands or lymph nodes may be a signal of an active or chronic infection that requires further attention. TMD(temporomandibular dysfunction) is a relatively common condition and has a variety of causes and possible solutions which should be discussed with your Dentist and Dental Hygienist. Often it is related to clenching, grinding (bruxing) of the teeth and some causes may include misalignment of your bite (occlusion), obstructive sleep apnea, or simply an increase in stress. Treatment planning may include referral to correct one or more underlying causes or if no treatable underlying causes are noted a Nightguard will likely be recommended to preserve the integrity of the teeth and jaw joints. A final and vital component of these bi-annual exams is the oral cancer screening. As your dental professionals we are charged with detecting suspicious oral lesions as we have more access than most patients’ physicians. If a lesion is detected a follow up visit will be scheduled to ensure that the lesion has resolved.
A beautiful, healthy smile not only contributes to a positive self-image, but it also helps to make a great first impression on everyone you meet. When you’re completely satisfied with the look of your smile, you’re likely to smile broadly and confidently more often.
If your teeth are stained, discolored, chipped, worn down, misshapen, a little gapped, or misaligned, you’re not alone. According to statistics, more than one-third of adults in the United States are dissatisfied with the appearance of their smiles. The good news is these days, you don’t have to be a movie star to have a vibrant and beautiful smile. Thanks to advances in cosmetic dentistry, less-than-perfect teeth can be completely transformed to produce a naturally beautiful looking smile.
Let us help you bring out the best in your smile!
At the office of Hawthorn Dental Associates, we offer a comprehensive range of state-of-the-art dental services and provide the highest level of personalized care. Our goal is to help every patient enjoy the benefits of an attractive smile. Whether you’re unhappy with the look of a single tooth, all your front teeth, or have unsightly gaps in your smile due to missing teeth, we can help.

Combining the art and science of dentistry
Even thousands of years ago, people were concerned about the health and appearance of their smiles. Viewing white teeth as a sign of wealth and beauty, the ancient Egyptians used small sticks to apply a mixture of ground pumice and wine vinegar to remove stains and whiten their teeth.
Today, we have the skills, technology, and materials to create smiles that are as beautiful as they are healthy. Thanks to developments in the field of cosmetic dentistry over the past 50 years, even the most challenging smiles can be transformed into ones that dazzle. At the office of Hawthorn Dental Associates, we offer state-of-the-art treatment along with an artistic eye and keen awareness of facial aesthetics to produce cosmetically pleasing smiles and long-lasting results of care.
You can rest assured your smile is in the best of hands with us. We value patient input and listen carefully to your interests and expectations of care. When it comes to cosmetic dentistry, there is no “one size fits all” solution. We recognize that every patient is unique and provide highly personalized treatments to enhance the look of your smile.
What Are Some Types Of Cosmetic Dental Procedures?
Cosmetic dental procedures range from treatments that are relatively quick and non-invasive procedures to more extensive ones based on a patient’s specific needs and expectations of care.
When staining, enamel defects, minor chips, small gaps, or slight misalignment are present, conservative and minimally invasive procedures such as cosmetic dental bonding, professional strength teeth whitening, and veneers can offer effective and highly satisfying ways to improve the look of your smile. Teeth with cavities, more extensive damage, or more significant cosmetic flaws, can be restored and rebuilt to achieve attractive, durable, and long-lasting results with tooth-colored fillings and natural-looking dental crowns.

Rebuilding a complete and beautiful smile
At the office of Hawthorn Dental Associates, we use leading-edge technology, proven methods of care, and the latest generations of dental materials to give patients the smiles they’ve always wanted!
We can also help patients with missing teeth to reestablish a complete and beautiful smile with options that range from dental bridges or dentures to dental implants. Whether an individual tooth or multiple teeth are missing, our practice offers the most advanced dental implant-based solutions to help patients create an attractive smile that looks, feels, and functions like a natural one.
Some of the most common cosmetic dental procedures we perform include the following:
-
Dental Bonding
To repair minor defects, chips, or fractures, mask discolorations, and close small gaps between teeth; a dental bonding procedure is considered one of the most effective, economical, and quickest methods of care. A bonding procedure is typically performed with composite resins, which come in a wide array of tooth-colored shades to enhance the look of your smile blend seamlessly with the rest of your teeth. Bonded to the underlying tooth structure, composite resins are made of biologically safe and metal-free materials that offer excellent aesthetics, strength, and durability.
-
Tooth-Colored Fillings
Today, it’s possible to restore a tooth with decay with cosmetically pleasing and metal-free filling materials composed of composite resin and filler particles that form a hard matrix when set. Strong and durable, these fillings bond to the remaining tooth structure as they rebuild it following the removal of any decayed or damaged portions. Best of all, with tooth-colored fillings, there’s no unsightly metal showing. Your smile looks naturally pleasing whether you’re opening your mouth or simply flashing a broad smile.
-
Teeth Whitening
If your teeth are stained, discolored, or yellowed, you may benefit from a professional strength teeth whitening procedure from our office. A teeth-whitening procedure can quickly transform a dull, drab, discolored smile into one that’s whiter and more vibrant. Although over the counter teeth whitening systems purchased in stores or online have become popular, there are health concerns and limitations with these products. As a rule, the healthiest and most effective methods of teeth whitening are the ones managed and supervised by the dentist. At the office of Hawthorn Dental Associates, we use the leading systems in care to offer a safe, quick, and effective way to lighten and brighten your smile!
-
Dental Veneers
One of the most conservative yet highly effective and aesthetically pleasing ways to enhance the appearance of imperfect looking teeth is the fabrication of porcelain veneers. By placing customized, ultra-thin facings made of the highest grade of dental porcelain over the front of a single tooth or multiple ones, our office can transform the look of your smile.
-
Crowns
Besides restoring the appearance and function of teeth with extensive dental decay, cracked fillings, prior root canals, or rebuilding teeth that are very worn down from grinding, a full coverage dental crown can also be used to improve the cosmetics of an imperfect tooth. A full coverage crown may be indicated for teeth that are misshapen, deeply stained, or otherwise significantly flawed.

Helping Patients Achieve Their Cosmetic Smile Goals
A successful and satisfying cosmetic treatment plan values patient input. As part of a cosmetic smile makeover consultation, your interests and concerns are discussed while your smile is carefully analyzed to determine which procedures will provide the most pleasing results of care.
Armed with a comprehensive knowledge of dental aesthetics as well as a thorough understanding of complex requirements of an optimally functional bite, the office of Hawthorn Dental Associates offers the treatment required to achieve your cosmetic goals and meet your expectations of care.
As skilled providers of cosmetic dentistry, we maintain a position at the forefront of advances in technology and dental materials to deliver the highest quality of care.
While the services described above reflect many popular options in care, we can also discuss additional procedures to improve the look of your smile.
Whether you’re looking to improve one tooth or many, it’s an excellent time to consider enhancing the look of your smile! For more information on cosmetic smile makeovers and the many dental services that we provide, give the office of Hawthorn Dental Associates a call today.
FAQs
+What is cosmetic dentistry?
Cosmetic dentistry offers solutions to improve the look of teeth that are stained, discolored, chipped, worn down, misshapen, a little gapped, or misaligned. It combines the art and science of dentistry to transform a less-than-perfect smile into one that looks naturally beautiful while at the same time enhancing overall facial aesthetics.
+What’s the quickest way to improve the look of my smile?
The great thing about cosmetic dentistry is that it offers multiple solutions to quickly improve the look of one’s smile. It all depends on your specific dental needs and cosmetic smile goals. While procedures such as teeth-whitening, tooth-colored fillings, and dental bonding typically provide dramatic improvements in just a single visit, others such as dental veneers only take a couple of visits.
+What’s the best way to improve the look of dull, drab, or discolored teeth?
A teeth whitening procedure as provided by our office is often the simplest, quickest, and most effective way to significantly lighten and brighten your smile.
+How can dental veneers improve the look of my smile?
Porcelain veneers are capable of concealing a range of imperfections, dramatically improving the look of teeth that are misshapen, have minor chips, enamel defects, or stains. They also provide an excellent solution for closing small gaps as well as addressing other minor alignment issues. While teeth whitening procedures can effectively treat many cases of dental stains or discolorations to produce cosmetically pleasing results, darker stains, as well as specific issues involving the size, shape, and alignment of the teeth, are better addressed with porcelain veneers.
+What type of cosmetic restoration is possible for a back tooth?
How a back tooth is repaired and restored depends on the extent of the cavity or damage it has sustained. In many cases, a tooth-colored filling is often sufficient to restore the form and function of a back tooth. However, when a significant amount of tooth structure is damaged, or the tooth has had a root canal, it’s often necessary to fabricate a full coverage crown. In this way, the remaining tooth structure is protected from further damage while full function and a natural- looking smile is restored.
+Does a tooth that is chipped require a crown?
Whether or not a chipped or fractured tooth requires a dental crown depends on the extent of the damage. Some minor chips can be addressed with a dental bonding procedure or a veneer. When a significant amount of tooth structure is lost, rebuilding the form and function of the involved tooth may require a full coverage crown.
+What the most cosmetic solution for replacing missing teeth?
While conventional dental bridges and dentures offer effective and satisfying ways to rebuild a complete and attractive smile, dental implants represent the most advanced solutions for replacing missing teeth. With dental implants, our office can replace a single tooth or multiple ones to give you a smile that feels, looks, and functions like a natural one. Dental implants behave in much the same way as the root of an actual tooth, providing stable, secure, and long-lasting results of care.
+How long does a tooth whitening last?
How long your teeth whitening lasts depends on your lifestyle. Eating, drinking, and smoking habits can have a big impact on maintaining your result. Our office will inform you which food, beverages, or habits can stain your newly whitened smile. As needed, we’ll also help you maintain a white and vibrant smile with a periodic, safe, and effective touch-up whitening procedure.
+How much do cosmetic dental procedures cost?
At the office of Hawthorn Dental Associates, we want every patient to enjoy the benefits of a beautiful and healthy smile. We strive to make dental care affordable and accessible. Improving the look of your smile is a worthwhile investment, and we always try to optimize any dental insurance benefits to cover your work. However, it’s essential to keep in mind that cosmetic dental procedures may not be covered by your plan. You can count on our office to explain every cosmetic option available to address your needs and the fees involved. To help you begin care without any additional stress or day, we can discuss different payment options and financing plans.
+Why choose the office of Hawthorn Dental Associates?
A beautiful smile begins today. For more information on our office or to schedule an appointment for a cosmetic smile makeover consultation, give us a call today.
If dental decay, cracked fillings, root canals, clenching or grinding the teeth have caused extensive damage to the underlying tooth structure a dental filling may not be a sufficient restoration. The only way to completely restore the cosmetic appearance and function of this tooth is often full coverage with a dental crown. The good news is that a completed dental crown looks and feels like a natural tooth.
In addition to restoring a single natural tooth, crowns can be used in other situations including being the supporting ends of dental bridge, covering dental implants, or as coverage for a cracked tooth to prevent further breakdown. A crown may also be indicated when a discolored or stained tooth needs to be restored to its natural appearance. Crowns can be made of either porcelain baked onto a metal substrate, all-porcelain, or many of the new ceramic materials that have been developed.
At the office of Hawthorn Dental Associates, we provide skilled and experienced care to help every patient enjoy the benefits of optimal oral health and a beautiful smile. For individuals who are missing teeth due to extensive decay, periodontal disease, trauma, the result of an illness, or side effect of medical treatment, we offer a comprehensive range of services to rebuild complete, attractive, and functional smiles.
How missing teeth impact the health and function of your smile
Missing teeth do more than cause embarrassing gaps in your smile. In the absence of a replacement, they can affect the health and function of your smile in the following ways:
- Impair your ability to smile, speak, and chew with confidence and ease.
- Allow the adjacent teeth to ever so slowly drift into the unoccupied spaces, thereby changing the alignment of your smile and bite.
- Cause teeth in the opposing arch that no longer occlude with a counterpart to extrude and further compromise your bite.
- Promote cavities and gum disease as the teeth shift out of place and impact the distribution of biting and chewing forces, and become more difficult to keep clean.
Rebuilding a complete smile
Although the consequences of missing teeth can compromise your dental health and overall well-being, modern dentistry offers effective solutions for reestablishing a complete, attractive, and well-functioning smile.
Today, thanks to advances in dental materials, technology, and treatment methods, it's easier than ever before to replace missing teeth and achieve aesthetically pleasing and long-lasting results.
Of course, each smile is different, and every patient has unique needs and individual expectations of care. Helping a patient rebuild a complete and beautiful smile may involve partial or full dentures, fixed dental bridges, or dental implants.
As skilled and experienced providers of care, the office of Hawthorn Dental Associates offers expert guidance on choosing the most suitable treatment option. Whatever type of tooth replacement method you select, you can feel confident that your smile will look good and feel great!
About dental bridges
A dental bridge offers a highly effective, stable, and fixed solution for replacing missing teeth. Unlike removable partial dentures that clasp on to the remaining teeth, a dental bridge relies on the support of crowns attached to teeth adjacent to the edentulous area (space without teeth) or strategically placed dental implants. In addition to restoring the look, feel, and function of a natural smile, they also prevent the teeth from shifting, thereby protecting the alignment of a patient's bite.
Far from a new idea, the history of replacing teeth with a fixed dental bridge goes back thousands of years. Ancient civilizations made impressive use of available materials, including animal and human teeth, bones, gold, and ivory, to fill gaps in a person's smile.
Fortunately, over the millennia, dental materials and technology have evolved. Today, dental bridges are fabricated from the highest quality of dental materials, including porcelain, porcelain fused to metal, and engineered ceramic products like zirconia. Now, in addition to being stronger and more durable than ever before, they appear more attractive and naturally beautiful.
Common types
Depending on the number of missing teeth, the health of the remaining dentition, and other factors, a dental bridge can replace a single missing tooth or multiple ones.
Although most resources list a traditional fixed bridge, an implant-supported bridge, a cantilever bridge, and a Maryland bridge as the four main types of bridges, the most commonly recommended ones are the first two.
-
Traditional fixed bridge
A traditional fixed bridge typically requires the preparation and crowning of teeth on either side of the edentulous space. These crowned teeth function to support the artificial ones, known as “pontics,” that span the gap. In much the same way a bridge that extends over a body of water relies on the support of strong, sturdy pillars at each end, a dental bridge garners strength and stability from the terminal crowned teeth fused to a single or multiple pontics.
Although related and similar to a traditional fixed bridge, a cantilever fixed bridge differs in one significant way. Only one side of the pontic will get attached to a crown for support.
-
Implant-Supported Bridges
As the most advanced method for the replacement of missing teeth, dental implants come the closest to replicating the look, feel, and function of a natural smile. For this reason, an implant-supported bridge often represents the best option in care.
With an implant-supported bridge, there's no need to prepare, crown, or involve any adjacent natural teeth. Because dental implants behave in much the same way as the roots of natural teeth, they provide all the support a bridge requires.
In addition to providing a self-supporting solution for the replacement of missing teeth, Implant-supported bridges offer the most versatile approach for rebuilding a complete smile. Strategically placed dental implants can support any number of replacement teeth up to an entire set of upper or teeth.
Furthermore, as dental implants provide the same stimulation as actual roots to the surrounding jawbone, implant-supported bridges also help prevent the bone shrinkage that naturally occurs when teeth have been lost. This feature helps maintain normal facial contours.
At the office of Hawthorn Dental Associates, our mission is to help every patient enjoy good oral health and the benefits of a beautiful smile. We provide skilled, experienced care and offer the most advanced dental implant-based solutions to transform incomplete smiles into ones that look great, function well, and inspire confidence.
Before a bridge gets fabricated
Successful treatment outcomes rely upon many things, including a careful assessment of a patient's oral health, overall well-being, smile goals, lifestyle, and budget. Whether you're a candidate for a traditional fixed bridge, an implant-supported bridge, or a removable denture will be determined following a comprehensive assessment and discussion with our office. We value patient input and strive to fulfill your expectations of care.
Before the fabrication and placement of a dental bridge, it's essential that your mouth is free from gum disease. If you have gum disease, it will need to get treated in advance of fabricating your bridge.
For traditional fixed bridges, the crowned teeth need to be strong and have sufficient bone surrounding them to offer strong support. Sometimes, a bone-grafting procedure to boost bone volume and provide a solid foundation is required before the fabrication of an implant-supported or traditional bridge.
At the office of Hawthorn Dental Associates, the care and comfort of our patients are our top priorities. Our goals are to create healthy and beautiful smiles and make every dental experience a positive one.
What to expect when getting a traditional bridge
Fixed bridges are typically fabricated over the course of multiple visits. The process involves the preparation of the supporting teeth, impression taking, the placement of a temporary bridge, and the try-in and cementation of the permanent restoration.
It begins with a complete diagnostic workup to develop an appropriate treatment plan. For patients getting a traditional fixed bridge, the next step in the procedure involves preparing the abutment (supporting) teeth for full-coverage crowns. Depending on the number of teeth involved and other factors, an impression for the permanent bridge can get taken this visit or the next one. Either way, a temporary bridge or temporary crowns to cover the prepared teeth will get placed to protect the prepared teeth.
Following the preparation of the involved teeth, it's not unusual to experience some sensitivity and gum soreness. This discomfort typically subsides. However, since the fit of a temporary restoration is often less precise than the final permanent crown or bridge, you may still feel some residual sensitivity until treatment is completed.
Until the permanent crown or bridge is placed, it's essential to be extra careful. Temporary restorations are far less durable than permanent ones. If your temporary gets damages or comes off, please hold on to it. Contact our office, and we will set up an appointment to replace it. Do not attempt to do this on your own.
Before cementing your new bridge, the shade, contours, fit, and occlusion are checked. Once that is done, your new, permanent restoration is placed. Since you have been wearing a temporary, your bite may feel slightly different, and you may feel some pressure as the new restoration reestablishes appropriate contact with the adjacent teeth. If the bite still feels slightly off after a couple of days or any discomfort persists, get in touch with our office. You may still require a minor adjustment.
What to expect when getting an implant-supported bridge
Surgery to place the dental implants is typically considered a minor surgical procedure and performed on an outpatient basis. However, the exact extent of the procedure depends upon the type and number of dental implants and whether or not any additional procedures are required to prepare the supporting bone.
As your trusted partner in care, you can count on our office to keep you well informed every step of the way. To facilitate the precise placement of dental implants for your implant-supported bridge, we'll take several detailed diagnostic records, including 3D images of your jaws and the involved area.
Patient care and comfort are our top priorities. We do everything we can to put you at ease and make every visit to our office both comfortable and stress-free. Prior to placing your dental implants, we'll discuss the anesthesia, options in dental sedation, and provide detailed pre-op and post-op care instructions.
Once the dental implants for your bridge are placed, it can take a few months for them to fully integrate with the surrounding bone. In some cases, a same-day temporary bridge can get placed to provide an immediate and cosmetically pleasing look. However, the permanent bridge typically gets placed when healing and osseointegration (fusion) with the surrounding bone are complete.
FAQs On The Topic Of Dental Bridges
+Will my smile feel any different?
Your new bridge is customized to the exact specifications of your smile. Before cementing to the underlying teeth or affixing it to the supporting implants, the shade, occlusion, and all aspects of its fit get carefully checked. In addition to being designed to blend seamlessly with your smile, it's also made to suit your bite and withstand all manner of oral function. We take great care to make sure your new restoration looks great, fits well, and that your bite feels comfortable.
+Does dental insurance cover the cost of a bridge?
Replacing missing teeth with a dental bridge is a worthwhile investment in the look, health, and function of your smile. While many dental insurances offer coverage for a dental bridge, and some toward the cost of implants, the benefits and amounts can vary significantly from plan to plan. At the office of Hawthorn Dental Associates, we understand the financial considerations involved in care and do all we can to help patients begin treatment without any additional stress or delay. In addition to doing our best to optimize your dental benefits, we also offer several payment and financing options. Feel free to contact our office if you have any questions on the cost of care, dental insurances, financing plans, or acceptable forms of payment.
+What’s the best way to care for my new bridge?
Now that your new permanent crown or bridge is in place, it's essential to maintain good oral hygiene. With proper care, your new restorations will last for years to come. Make sure to brush and floss as instructed. We'll show you how to floss under your dental bridge to keep your new smile clean and bright. Remember to make appointments for your routine checkups and professional cleanings.
+How long can a bridge last?
The standard answer is that with routine dental visits and good home care, a bridge can last ten to fifteen years, and in many cases, much longer.
+Why choose our office?
At the office of Hawthorn Dental Associates, we fabricate your bridge from the highest quality dental materials to achieve the most cosmetically pleasing and lifelike results of care. It's also customized to the exact specifications of your smile and designed for optimal aesthetics, strength, and stability. Once fabricated and cemented into place, you'll feel confident sharing your smile, speaking, and eating your favorite foods.
As your trusted partner in care, we analyze every aspect of your smile to develop a treatment plan that provides aesthetically pleasing, healthy, and long-lasting results of care.
For more information on dental bridges, or any services we provide, give us a call today.
Restoring Teeth With Dental Fillings
When dental decay compromises a tooth's structural integrity, a filling gets placed to rebuild its natural form and restore its strength and function.
Because tooth decay, also known as dental caries, remains one of the most prevalent chronic diseases affecting both children and adults worldwide, procedures to place fillings are routinely performed each and every day.
At the office of Hawthorn Dental Associates, we provide precise and gentle treatment and maintain a position at the forefront of advances in care to provide patients with the highest quality of aesthetically pleasing and durable dental fillings.
The History Of Dental Fillings
According to archaeological findings, for as long as dental problems have existed, there have been efforts to provide emergency and restorative care. In fact, attempts to place dental fillings have been found in the skeletal remains of people who lived around the year 8000 BC. However, it wasn't until thousands and thousands of years later, in the 19th century, that a variety of metal fillings, including dental amalgam, appeared on the scene. Although gold achieved status as a popular restorative material, it was soon apparent that amalgam fillings, consisting of a mixture of mercury and an alloy composed of silver, tin, and copper, offered a less expensive, durable, and simpler alternative.
Until recent decades, the vast majority of dental fillings remained silver-colored, amalgam restorations. However, as dentistry has evolved in the last 50 years, new filling materials have been developed. While amalgam fillings are long-lasting and durable, today's newer materials offer the benefits of being mercury-free, metal-free, and much more aesthetic. These "tooth-colored or white fillings" invisibly restore the form and function of the involved tooth, while seamlessly blending in with the remaining tooth structure and the entire smile.
Our Commitment To Restoring Oral Health And Beautiful Smiles
At the office of Hawthorn Dental Associates, we tailor treatment to address specific dental needs and expectations of care. As with all the services our practice provides, we'll explain all your options in care, including the type of dental filling materials we offer to restore your tooth. Our goals are to gently remove the dental decay and the damaged tooth structure and then rebuild your tooth's form and function while providing you healthy, durable, long-lasting, and cosmetically pleasing results.

What are the different types of dental fillings?
While traditional dental materials like gold and amalgam have been in use for over a century, recent advances in dental technology have made a more expansive and improved selection of restorative choices widely available. Beyond offering strength and durability, these new filling materials provide aesthetically pleasing and natural-looking results.
Some commonly used filling materials include the following:
-
Composite Fillings
Composite fillings, which are frequently referred to as either "tooth-colored fillings" or "white fillings," consist of a combination of biocompatible resins and finely ground, glass-like filler materials that become strong and durable when set. Available in a complete range of natural-looking shades, composite fillings offer a cosmetically pleasing alternative to traditional "silver" fillings. Composite resins are also used in dental bonding procedures to improve a tooth's color or shape, mask defects, or close minor gaps between teeth.
Composite fillings adhere to natural tooth structure through a bonding process, which also serves to seal and strengthen the tooth. Beyond providing a close match to your natural tooth color, a composite filling does not require removing of as much tooth structure for placement, nor are they subject to expansion or contraction with temperature changes as is the case with dental amalgams. However, composite restorations can be more vulnerable to wear and staining and may require replacement down the road.
-
Silver Fillings (Amalgam)
For many years, amalgam fillings represented the standard of care for restoring decayed teeth. While they don't offer the cosmetic appeal of other types of filling materials, amalgam restorations are strong, durable, and less likely than some other types of fillings to break or wear down.
-
Glass Ionomers
Another type of white filling material, glass ionomer cements bond to the tooth's surface to provide a tight seal between the tooth and surrounding oral environment. Besides offering a natural-looking restoration, glass ionomer cements slowly release fluoride to strengthen and help protect the involved tooth from future decay. Since they are not as durable or wear-resistant as other filling materials, glass ionomers are most frequently used to treat baby teeth, cavities near the gumline, and in temporary fillings.
-
Ceramic Fillings
Ceramic fillings, inlays, and onlays are fabricated from the highest quality of dental porcelain and ceramics. As the most stain and wear-resistant option in tooth-colored fillings, these restorations offer durable, attractive, and long-lasting results. While "direct" fillings such as dental amalgam and composite fillings get placed immediately after the tooth is prepared, "indirect" fillings such as inlays or onlays get fabricated outside of the mouth before insertion and cementation or bonding.
-
Gold Fillings
Far less common these days and more expensive than any of the other materials, gold fillings remain excellent restorations. With excellent physical and chemical properties, gold fillings are strong, long-lasting, kind to the surrounding tissues, and remain stable over time.
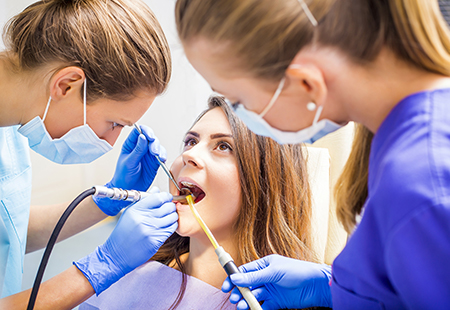
How are cavities treated?
Once our office has a chance to assess your smile, we'll advise you of our findings and outline a comprehensive treatment plan to help ensure your smile is healthy and functions at its best. If any tooth decay is detected, we'll schedule appointments to treat those cavities and place the fillings or restorations that are needed.
At the office of Hawthorn Dental Associates, patient care and comfort are our top priorities. While treating cavities and placing fillings are among the most routine procedures in dentistry, our office understands you have questions and concerns and will keep you well informed every step of the way.
Treating a cavity involves the precise and gentle removal of decayed and damaged tooth structure and any preparation of the remaining tooth structure needed to secure your new filling. Although every patient and every smile is different, you can expect your visit to take about an hour.
In most cases, this visit is performed under local anesthesia. As the work gets performed, your tooth is completely numb, and you should not feel any discomfort. A dental drill, dental laser, or air abrasion technology can be used to remove decay. Once the cavity gets excavated, and healthy tooth structure remains, it's time to place the filling. The type of dental filling material being used determines the manner of placement. Composite fillings, glass ionomer cements, and amalgam fillings are typically placed right away. However, in the case of an extensive cavity, a tiny palliative dressing and a temporary filling may be placed. Whatever type of filling is used, our office will check the fit, do any necessary polishing, and meticulously adjust the bite to ensure your optimal comfort and function.
For patients who are anxious about dental work, you can rest assured the office of Hawthorn Dental Associates is mindful of your needs. As skilled and experienced providers of care, we pride ourselves on providing gentle dentistry and do all we can to make your visit comfortable and stress-free. While we perform dental procedures under local anesthesia, we're also happy to discuss options in dental sedation.

What Do I Need To Know Following The Placement Of My New Filling?
At the office of Hawthorn Dental Associates, our goal is to help our patients enjoy optimal oral health and to keep them well informed every step of the way.
Immediately after the placement of a new filling, it's essential to keep the following in mind:
-
Until the anesthesia wears off
Immediately following your dental visit, you may experience a period of lingering numbness. Normal sensation typically returns within an hour or two. However, until the anesthetic has completely worn off, it's essential to protect yourself from unintentionally biting or injuring your lips, cheeks, gums, or tongue. Be mindful of chewing, drinking hot beverages, or smoking. -
Now that your tooth has been restored and rebuilt, it may feel slightly different
While we take the utmost care to polish your new filling and make sure the bite is correct, on rare occasions, a patient may feel additional minor smoothing or further bite adjustment is required. -
You may experience short-term sensitivity
It's perfectly normal for a tooth to feel a little sensitive following the placement of a filling. You may experience a twinge when eating cold or hot foods and beverages. This sensitivity should subside by itself within a few days. If your sensitivity worsens, you experience ongoing pain or develop any other symptoms; please contact our office. -
Caring for your new restoration
Our office uses the latest generations of strong and durable filling materials. With proper oral hygiene and routine care, your new filling should last for many years to come. However, in cases of extensive tooth decay or injury to the underlying tooth, even the best restoration may need to be replaced, or further dental work may be needed down the road.
We're passionate about what we do and dedicated to providing the highest quality of care. If you have any additional questions or concerns, feel free to contact our office.
FAQs On The Topic Of Dental Fillings
+Are my teeth just sensitive, or do I have a cavity?
If the pleasure of eating a delicious bowl of ice cream or sipping a soothing cup of tea gets overshadowed by dental pain that makes you wince; it's time to contact our office. As skilled providers of care, we'll determine what's causing your discomfort and perform the treatment required to alleviate your symptoms and get you back on the road to oral health.
+What causes a cavity to develop?
Cavities develop because of an infectious process that causes progressive damage to tooth structure. Despite starting as a pinpoint defect on the outermost enamel layer of your tooth, untreated dental decay progressively compromises more and more healthy tooth structure as it works its way to the inner layers of your tooth.
+Can I still get a cavity if my tooth already has a filling?
Yes, you can still develop tooth decay on other surfaces of the tooth, around the margins of an old filling, or in fewer instances, recurrent decay underneath it. For this reason, it's essential to maintain excellent oral hygiene, a diet low in sugary beverages and sweets, and be sure to visit our office for routine checkups and care. While tooth decay is second only to the common cold in frequency, it's almost entirely preventable.
+Is it possible to have more than one filling done at the same visit?
We value the time and comfort of our patients. If cavities are located on adjacent teeth, or in the same section of your smile, it may be possible to treat more than one tooth during your visit. However, how much is done each visit depends on several factors. We keep our patients well informed and tailor every treatment plan and visit to address their unique needs.
+Are silver amalgam fillings safe?
Addressing concerns on the presence of elemental mercury in silver fillings, the American Dental Association (ADA), The Center for Disease Control and Prevention (CDC), the FDA, and the World Health Organization have all stated that amalgam restorations do not pose a risk to health. However, individuals with allergies or sensitivities to the metals in dental amalgam are advised to pursue other restorative options.
+Does it hurt to get a filling?
Dental fillings are performed under local anesthesia to help ensure your comfort throughout the entire procedure. The involved tooth remains completely numb for the extent of your visit. Within one or two hours after the procedure is completed, the local anesthetic will gradually wear off, and normal sensations return.
+When can I eat after my visit?
A tooth-colored composite filling is fully hardened and set by the end of your visit. However, we may advise you to wait a couple of hours until the local anesthesia has completely worn off. This advice is to help ensure you don't accidentally bite your lip, cheek, or tongue while still numb.
+How long do dental fillings last?
The lifetime of a dental filling varies depending on the type of material used. While popular dental materials can last a decade or more with proper care, they can degrade over time, wear down, or even break. When this happens, you may experience some tooth sensitivity, a jagged edge, or a loose or dislodged piece of filling material. Whatever the case may be, it's essential to get the filling replaced before the tooth sustains further damage or other consequences arise. Beyond taking good care of your smile we can help ensure the longevity of your fillings, our office regularly checks the status of your existing fillings as part of a routine checkup exam.
+How much do fillings cost?
Dental fillings are an essential investment that serves to preserve and protect the health of your smile. With that said, how much a filling costs depends on the number of surfaces of the tooth involved and the filling material that is used. Amalgam restorations are the most economical. While tooth-colored composite fillings have a slightly higher cost, they offer the added benefits of being metal-free and much more aesthetically pleasing. Ceramic fillings, inlays, and onlays are more expensive than the preceding options but provide outstanding, long-lasting, and natural-looking results.
+Does dental insurance cover the cost of getting a filling?
Dental insurances typically cover the cost of dental fillings. While we work with you to maximize your insurance benefits, there may still be an out-of-pocket expense. At the office of Hawthorn Dental Associates, we strive to help you begin care without any additional financial stress or delay.
Thanks to advances in dental materials, technology, and methods of care, it’s easier than ever before to replace missing teeth with the most natural-looking and aesthetically pleasing treatment outcomes. While dental implants and fixed bridgework provide effective and satisfying solutions for missing teeth, removable dentures remain a tried and true method for reestablishing a complete smile.
At the office of Hawthorn Dental Associates, we fabricate dentures from the highest grade of dental materials for a precise and comfortable fit. Our dentures are meticulously designed to rebuild beautiful smiles and support natural facial contours while enabling patients to speak, smile, and chew with renewed confidence and ease.
We’re dedicated to helping patients to enjoy the benefits of a beautiful smile and take pride in offering personalized solutions to address their dental needs, lifestyle, and budget.
How missing teeth affect your smile, your health, and your outlook
According to recent statistics, it’s estimated that across the country, over 175 million adults have lost at least one tooth, and close to 40 million are missing all of their teeth. In most of these cases, tooth loss is the end result of extensive dental decay, advanced gum disease, a traumatic injury, a congenital anomaly, or associated with a medical condition.
In addition to the psychological and social consequences having embarrassing gaps in your smile often produce, missing teeth can affect your ability to speak clearly and eat a satisfying and nutritious diet. Left unaddressed, missing teeth can also cause gradual changes to your appearance and the alignment of your remaining teeth. These changes not only affect your bite, but they have the potential to create more unsightly and unhealthy gaps in your smile. Furthermore, without the support of a complete set of teeth, facial contours may also begin to look more sagged and haggard over time.
While it’s never too late to rebuild a complete and beautiful smile, it’s always best to replace missing teeth sooner than later. Both partial and full dentures from the office of Hawthorn Dental Associates offer an effective and satisfying solution for reestablishing a complete smile.

What are dentures?
Dentures are removable appliances that are designed to precisely and comfortably rest on top of the gums that cover the jawbones. They consist of natural-looking artificial teeth set in a supportive base. In addition to offering a cost-effective solution for the replacement of missing teeth, dentures are quite versatile. They can be used to replace either a few teeth that have been lost or all of the teeth in the upper or lower jaws.
While conventional bridgework and dental implants offer fixed solutions for rebuilding complete smiles, partial and full dentures are removable oral appliances. This statement means it’s possible to take dentures out of the mouth to clean and maintain the health of the underlying tissues and any remaining teeth, as well as clean the dentures themselves, or remove them while sleeping.
Types of Dentures
You can rest assured that rebuilding your smile is in the best of hands at the office of Hawthorn Dental Associates. As skilled and experienced providers of care, we’ll carefully evaluate all aspects of your smile, the health and integrity of any remaining teeth, along with the surrounding tissues and the supporting bone to develop a treatment plan that satisfies the functional and aesthetic requirements of your case.
The two main types of removable dentures are full dentures and partial dentures. Which of these types offers the best solution for your smile depends on how many natural teeth are still present in your mouth and the health of these remaining teeth. While a partial denture can offer an effective solution in cases where some sturdy natural teeth remain, you may be a candidate for a complete denture when all the upper or lower teeth are missing or require extraction.
Full Dentures
Full dentures, also known as complete dentures, can effectively replace all the upper teeth, lower teeth, or both the upper and lower teeth. As with other types of dental solutions, there’s no one-size-fits-all approach for every case. The ultimate design, fabrication, and insertion of a full denture can vary based upon a patient’s specific needs.
Conventional Full Denture
This type of denture is fabricated and placed after all of the remaining teeth are removed, and the surrounding tissues have adequately healed. Fabricating a full denture when healing is complete supports a precise and comfortable fit.
-
Immediate Denture
With an immediate denture, a patient does not have to go without teeth while waiting for complete healing of the extraction sites. Although an immediate denture offers the advantage of not having to go without teeth for any length of time, it can require a reline and adjustments as the tissues remodel and heal. In some cases, for optimal comfort and fit, a conventional denture may eventually be required.
-
Overdenture
An overdenture is a type of complete denture that receives added stability and support from special attachments that are secured to the remaining underlying teeth or specialized dental implants.
-
Implant-Supported Dentures
As the name implies, this type of denture attaches to a select number of strategically placed implants in the upper or lower jaw. These small surgical posts provide precise points of attachment for the overlying denture and add a significant measure of stability and retention.
Partial Dentures
In situations where some sturdy teeth remain, partial dentures can offer an effective solution for the replacement of missing teeth. Partial dentures typically achieve adequate retention and stability with clasps or precision attachments on the teeth adjacent to the edentulous areas (the spaces formerly occupied by the missing teeth).
Removable partial dentures can fill the void left by individual missing teeth and multiple ones to restore the look and function of a complete smile. At the same time a partial denture fills the gaps left by missing teeth; it also stabilizes the dentition and bite and prevents unwanted drifting of the remaining natural teeth.
As with full dentures, partial denture design and fabrication varies based on a patient’s specific needs. With advances in dental materials and technology, partial denture wearers have more options than ever before. Today, a partial denture’s supportive framework can be fabricated from various materials, including cast metal, flexible resins, and hybrid materials.
At the office of Hawthorn Dental Associates, we’re dedicated to building healthy and beautiful smiles. As your trusted partner in care, you can depend on our office to design and fabricate a denture that will look good, fit comfortably, and serve you well for years to come.

Providing integrated solutions to rebuild smiles
Fabricating an attractive, well-fitting, and long-lasting denture requires a comprehensive understanding of oral function, facial aesthetics, dental materials, and appliance design. At the office of Hawthorn Dental Associates, we maintain a position at the forefront of advances in care and successfully combine the art and science of dentistry to provide patients with outstanding treatment outcomes.
Once we’ve had an opportunity to review your medical and dental history, assess all aspects of your smile, and discuss your expectation of care, we’ll discuss the best options for restoring and rebuilding your smile.
Based upon a comprehensive analysis of your case, including advanced diagnostic imaging, we’ll advise you if any dental work, additional procedures, or extractions are required prior to the fabrication of a partial or complete denture. It’s essential that any remaining teeth are healthy and have sufficient bone support. Sometimes, a pre-prosthetic procedure to improve the tissue anatomy and ensure a denture’s optimal fit is recommended.
Having a denture or set of dentures made is a sophisticated process involving dental impressions, framework try-ins, selecting the right shade, shape, and size of the artificial teeth, and making sure that the bite and all aspects of oral function are comfortable and healthy. Whether it takes a single visit or a few visits to fabricate a partial or complete denture, a satisfying and healthy outcome relies on the careful execution of every step in care.

What To Expect When You Receive Your New Denture
At the office of Hawthorn Dental Associates, our patients' care and comfort are our top priorities. Our goal is to help patients enjoy optimal oral health and to keep them well informed every step of the way.
-
Adjusting to wearing a new denture
Getting used to wearing a new denture, especially a full denture, can take a little time. It’s not unusual to need some minor adjustments as you begin to speak, chew, and function with your new teeth. It can take a few adjustments to fit completely and feel comfortable. If you have a sore spot, try to wear the denture at least the day before your adjustment visit. In this way, we can see exactly where we need to relieve the area causing your irritation.
-
More saliva than usual
One of the natural responses to a new denture is for your mouth to produce more saliva. Not to worry, this is only a temporary reaction. The flow of saliva gradually decreases back to a normal level.
-
Speaking with ease
While it may seem challenging to speak clearly at first with a new denture, that feeling will pass within a few days. It’s important to keep talking, as usual, to allow yourself to adapt to your new set of teeth. You can help things along by reading some passages from printed materials or a computer out loud. -
Getting used to eating with a denture
If this is your first denture, it can also take some time to adapt to eating with your new prosthesis. Getting used to eating with a full denture is typically more challenging than doing so with a partial denture. It’s best to start with soft foods and to avoid chewing on just one side. Your tongue, lips, cheeks, and soft tissues will soon adapt to chewing with your new denture, and from then on, you’ll be able to eat with ease.
-
Taking care of your dentures
-
It’s essential to keep your denture clean! Rinse your dentures after eating and brush them daily. In this way, you can prevent stains and bacteria from accumulating on your new set of teeth. It helps to use a brush designed for dentures. Also, remember to soak your dentures in water when you’re not wearing them and at least once a week in the recommended denture cleaner.
-
Brush any remaining teeth as well as your gums to keep them clean and the tissues healthy and firm. If you wear an upper denture, rinse and gently clean the roof of your mouth as well.
-
Take your dentures out at bedtime. This practice gives the gums and the jawbone a chance to rest, helping to prevent irritation and infection as well as bone resorption (shrinkage).
-
-
Added stability
Due to the status of the underlying tissues and other factors, there are some cases where full dentures benefit from additional means of retention. While denture adhesive is often sufficient, full dentures that are implant-supported or clip onto special attachments offer added stability and retention.
-
Follow-up care
Maintaining oral health and overall well-being involves routine checkups and care. At these visits, we not only check the fit and condition of your dentures but we also perform a comprehensive exam to check the status of any remaining teeth as well as assess the health of all of the soft and hard tissues in and around the oral cavity.
-
Relines
Over time, the tissues supporting the denture can change. As the shape and contours of these tissues shrink or remodel, your denture may not fit as comfortably or feel as stable as it once did. A separate procedure, which is known as a reline, may be recommended.
At the office of Hawthorn Dental Associates, we’re dedicated to providing the highest quality of care. If you have any additional questions or concerns about your new dentures, feel free to contact our office.
FAQs
+What the best way to replace missing teeth?
Today, it’s easier than ever to replace missing teeth and achieve natural-looking, durable, and long-lasting results! Depending a patient’s dental needs, lifestyle, expectations of care, and budget, choices can include conventional fixed bridgework, dental implants, or removable partial and complete dentures. At the office of Hawthorn Dental Associates, we’ll discuss all your options in care and answer all your questions as you choose the solution that’s right for you.
+Do dentures provide natural-looking results?
With advances in dental materials and technology, today’s dentures are more comfortable and realistic-looking than ever before.
+Do I still have to see a dentist if I wear dentures?
Whether you wear partial or complete dentures, it’s essential to see the dentist for routine care. Besides checking the fit and condition of your dentures and making any necessary adjustments, you’ll also receive a comprehensive exam to check on the health of any remaining teeth as well the soft and hard tissues in and around the oral cavity.
+What’s a same-day denture?
A same-day denture offers an accelerated design and fabrication process that allows a patient to go from impression taking to denture insertion in a single day.
+What is the main benefit of an immediate denture?
For patients who don’t want to wait after having teeth extracted, an immediate denture can be inserted the same day your teeth are removed. Sometime later you may need the denture reline to address any changes in its fit once the extraction sites have completely healed.
+What if I break my denture?
While no one wants to drop or break a partial or complete denture, accidents do happen. The good news is that in some cases, your partial or complete denture is reparable. It all depends on the extent of the damage. Don’t hesitate to contact our office if you’ve broken or damaged your denture. We’re happy to help.
+What if the clasps on my partial have loosened?
The simple act of taking your partial denture in and out can cause certain types of metal clasps to loosen over time. When you come in for your checkup visit or contact our office for an adjustment, we’ll assess the fit of your partial and tighten the clasps for improved stability and comfort.
+How much do partial or complete dentures cost?
While rebuilding a complete smile is a worthwhile investment, our office is sensitive to the costs involved in dental care. We customized care and will discuss which treatment options address your needs, lifestyle, and budget. How much a new denture will cost depends on the type of the prosthesis, its design, and the materials used to fabricate the supportive base, teeth, and clasps or precision attachments. Dentures that include the placement of dental implants for added retention and stability typically involve additional costs.
+Does dental insurance cover the cost of dentures?
If you have dental insurance, your coverage may include a new or replacement set of dentures. Our staff is happy to review your coverage with you to ensure you are maximizing your insurance benefits while minimizing any out of pocket expenses.
+Why choose the office of Hawthorn Dental Associates?
At the office of Hawthorn Dental Associates, we provide an extensive range of dental services, including the latest and most effective methods to help patients with missing teeth rebuild complete and beautiful smiles. As skilled and experienced professionals, we recognize that every patient is different, and every smile is unique. We’re passionate about what we do and take great pride in providing personalized treatment plans while treating our patients as valued partners in care.
Are You Looking For An Emergency Dentist In Vernon Hills?
Whether you or any member of your family are suffering from a chipped tooth, toothache, wisdom teeth issues, or other problems affecting your oral health, you can be sure to get the prompt attention and skilled care you need at the office of Hawthorn Dental Associates.
While emergency dental care is a service we hope you'll never need, Hawthorn Dental Associates can help! As anyone who has ever had a toothache or sustained a dental injury can attest, the experience is both painful and upsetting. Although getting some measure of relief is a paramount concern, timely care is critical to prevent further consequences to your oral health and overall well-being.
At Hawthorn Dental Associates, our experienced, compassionate dental team provides a broad range of services to address dental emergencies in Vernon Hills and the surrounding communities. We can assure you that your smile is in the best of hands with us. Patient care and comfort are our top priorities. Our practice maintains a position at the forefront of advances in diagnostic and treatment technology to provide precise, gentle, and safe care.
We treat many types of dental emergencies and urgent oral health problems, including:
- Toothaches
- Chipped or fractured teeth
- Abscesses
- Loose or broken fillings
- Dislodged or lost dental crowns
- Broken, ill-fitting, or lost dentures
- Problematic wisdom teeth
- Acute Periodontal Problems
- Loose or broken down teeth
- Swollen, bleeding gums
- Bacterial, viral, or fungal Infections affecting the tongue, cheeks, gums, lips, or other soft tissues of the mouth
- Oral pain or swelling of unknown origin
- Suspicious bumps, spots, and lesions

Let Hawthorn Dental Associates Help Alleviate Your Discomfort and Restore Your Oral Health
Our goal is to get you back on the road to oral health as quickly as possible. As a trusted emergency dentist, you can count on our office for prompt, skilled, and reliable care.
Treatment for dental problems such as a toothache or a fractured tooth can vary. It all depends on the extent of the damage caused by the decay or trauma. Care may involve the placement of a new dental filling, dental bonding, or a larger restoration such as a crown to rebuild the tooth's form and function. If the damage has reached the tooth's nerve and vital inner tissues, you may need root canal treatment to save your natural tooth. Root canal treatment is a highly effective procedure with a greater than 95% success rate. Although we provide leading-edge care and do all we can to help save your tooth, in some situations a dental extraction is required. While losing a tooth can feel a little overwhelming, there's no reason for despair.
With advances in dentistry, there are several options available for the replacement of missing teeth, including dental implants, conventional fixed bridges, and partial or complete dentures. Today, dental implants represent the most advanced method for replacing a lost tooth and reestablishing a complete and beautiful smile.
Frequently Asked Questions
−What is a dental emergency?

Toothaches
Pain is your body's way of signaling that something is not quite right and though there are many reasons for oral pain, one of the most common complaints and reasons for seeking urgent dental care is a toothache. Whether you simply need a dental filling, a crown, or require a root canal procedure to save your tooth, we'll alleviate your discomfort and restore the look and function of the involved tooth.
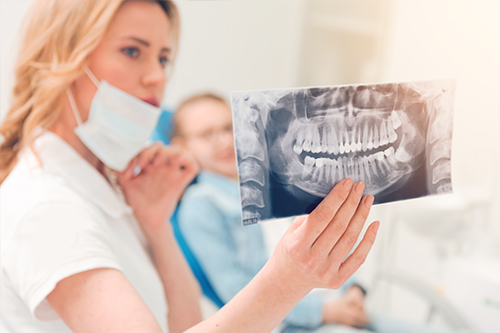
Dental Trauma
Dental trauma can result in a defect as minor as a small chip in tooth enamel to a more extensive and painful crack or fracture. With sufficient force, a tooth can even be displaced or completely knocked out of its socket. With prompt emergency care, many injured teeth can be restored and saved.
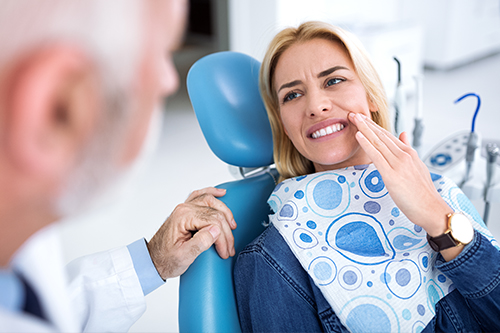
Wisdom Teeth
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall well-being. Our office provides skilled care to address the complications caused by problematic wisdom teeth.

Broken or Lost Dental Appliances
A broken or lost dental prosthesis or restoration can cause embarrassing gaps in your smile as well as compromise your ability to eat and speak with ease. If you've lost or broken a dental filling, denture, crown, or other dental appliance, you can rely on our office to perform a prompt repair or provide a durable and cosmetically pleasing replacement as quickly as possible.
At Hawthorn Dental Associates, emergency appointments are always available. Of course, in addition to providing top treatment for dental emergencies, we also welcome patients searching for high quality and affordable care. We offer a complete range of the latest and best cosmetic and dental services for every member of your family.
+How long do I have to wait for an emergency dental appointment?
If you are suffering from a toothache or have sustained a dental injury, it is important to visit the dentist as soon as possible before more serious complications arise. Whether your dental emergency is painful, if it affects the appearance of your smile, or if you suspect that an infection is present, our office will make every effort to see you as promptly as possible for care.
At Hawthorn Dental Associates, we treat your dental emergency as our top priority. Our caring team will respond to your emergency call right away, making sure you get the gentle, state-of-the-art care you need without delay.
As your trusted emergency dentist in Vernon Hills, we provide the highest quality of care to mitigate the stress, anxiety, and discomfort of dental problems. Our dedicated team will help you start feeling better as soon as we receive your emergency call.
+Do I need to go to the emergency room or hospital?
At Hawthorn Dental Associates, we provide skilled and experienced care to effectively resolve a broad range of dental emergencies, restoring a patient's oral health while protecting their overall wellbeing.
However, even so, specific dental emergencies pose significant threats to one's health. These situations require immediate, emergency room care. Serious and potentially life-threatening dental emergencies include significant oral and facial trauma such as jaw fractures, deep wounds or lacerations to the face and mouth, an abscess or infection that causes widespread facial or submandibular swelling, or affects breathing and swallowing.
+How much does emergency dental treatment cost?
At Hawthorn Dental Associates, we provide prompt, skilled, and experienced care to address dental emergencies. We understand that finances are always a concern and do our best to provide options in care that are both affordable and respect your budget.
Once we've had the opportunity to examine your smile, we can give you a clear picture of any existing dental issues, along with a quote for what the cost of treatment will be. The cost of care all depends upon the extent and complexity of issues affecting the health or appearance of your smile and the types of procedures that are required.
To help alleviate any additional stress or delay, you can count on our staff to work with you to optimize coverage for your dental care and to minimize your out-of-pocket expenses. For patients without insurance, we strive to make things easier as well! We invite you to visit our financial information page or speak to an expert in our business office.
+Why Choose Hawthorn Dental Associates For Your Emergency Dental Treatment In Vernon Hills?
Dental emergencies are often painful and debilitating experiences. For this reason it's important to have an emergency dentist in Vernon Hills, who welcomes patients with urgent dental needs while providing the prompt care required to restore oral health.
Here are just some of the reasons why so many patients choose our office for emergency dental care and to meet their family's dental needs:
- Skilled and compassionate care for patients of all ages
- Ultra-modern office designed with patient comfort in mind
- Professional team experienced in all facets of care
- State-of-the-art diagnostic and treatment technology
- Precise and gentle treatment using leading-edge systems of care
- Careful attention paid to patient input and treatment expectations
- Detailed explanations of treatment options and every step in care
- Provision of a broad range of dental services and emergency procedures
- Recognizes the specific needs of each patient and the unique requirements of every smile
- Provide patients with the education and tools to establish a strong foundation for optimal oral health
We're dedicated to helping patients enjoy good oral health and beautiful smiles. We look forward to helping you keep your smile in tip-top condition. You can rest assured that our highly skilled office team will provide you the highest quality of state-of-the-art dental care and have you smiling again in no time!
To make an appointment or for more information on our office and the many state-of-the-art services we provide, give us a call today.
At Hawthorn Dental Associates, We Provide Care To Support Ongoing Oral Health And Help Prevent Dental Emergencies
While some dental emergencies cannot be predicted or avoided, practicing good oral hygiene, a healthy diet, and routine care go a long way to protect the health of your smile.
At Hawthorn Dental Associates, we emphasize taking a preventive approach to care to help you and every member of your family maintain healthy, beautiful smiles. By coming to our office as recommended for checkup visits and routine care, we can help to prevent both the onset and progression of many oral health problems. We offer a comprehensive program of preventive care, including examinations, professional teeth cleanings, and oral cancer screenings, along with patient education on hygiene, diet, and healthy practices.
Your oral health and overall well-being are our top priorities. Remember, it's best not to hold off seeing the dentist until you're in terrible pain or think there's something wrong. By scheduling a routine appointment for a comprehensive checkup, a professional cleaning, and routine dental care, our skilled dental team can help you keep your smile looking and functioning its very best.
What You Need To Know About Having A Tooth Extracted
At the office of Hawthorn Dental Associates, our patients' care and well-being are our top priorities. Every member of our skilled and experienced team strives to ensure patient comfort and a stress-free dental experience. Our dedication to the consistent provision of compassionate and personalized attention along with gentle, precise care has earned our office the respect and trust of our patients.
While we do everything we can to preserve the integrity of your natural smile, it's sometimes necessary to extract a tooth to protect your oral health and overall well-being.
Some of the most common reasons our office may recommend having a tooth extracted include the following ones:
-
A "baby" or deciduous tooth that is over retained (reluctant to fall out), severely decayed, or damaged
In most cases, a baby tooth will fall out as scheduled as the underlying permanent one begins to erupt into place. However, occasionally a baby tooth continues to remain firmly attached to the bone. Either the roots of the baby tooth have failed to resorb and shrink as intended, or the baby tooth has become anklylosed and fused to the supporting bone. The problem is that over-retained baby teeth can disrupt the development and alignment of your child's smile. As we monitor your child's smile as they grow, we'll advise you if and when an extraction of a baby tooth is required to facilitate the eruption of its underlying permanent successor. -
A permanent tooth that has extensive decay and is deemed non-restorable
Beginning as a simple pinpoint defect on the outermost enamel layer of your tooth, untreated dental decay will continue to compromise healthy tooth structure as it works its way to the inner layers of the tooth. Without proper care, a cavity can lead to significant damage to tooth structure, irreversible damage to the nerve of the tooth, a dental infection, and serious consequences to your oral health and overall well-being. When the tooth has sustained far too much structural damage and cannot be restored, a dental extraction may be required. -
A permanent tooth that has been severely fractured or cracked and can not be restored
There are many different types of chips, cracks, and fractures that can affect your teeth. The extent of the damage that it causes will determine if there is enough intact tooth structure to save the tooth and the type of treatment required. In cases where too much tooth structure or the root of a tooth has also been compromised, an extraction may be necessary. -
Advanced gum disease that has significantly compromised the tooth's supporting tissues
The most common cause of tooth loss in adults is gum disease. When left untreated, periodontal disease, which affects the hard and soft tissues supporting your teeth, can lead to gingival pocket formation, gum recession, and diminishing alveolar bone. As advanced and untreated gum disease progresses, the teeth ultimately loosen, fall out, or require extractions. -
Poorly positioned, impacted, or decayed wisdom teeth
Wisdom teeth, which are also known as the third molars, are the last permanent teeth to develop in the oral cavity and the final ones to come into place. However, as is often the case, many wisdom teeth do not have sufficient room to erupt, are not developing correctly, develop extensive decay, or cause issues for the adjacent teeth and the surrounding tissues. Although the extraction of wisdom teeth sometimes gets recommended for an older patient, the early removal of troublesome or potentially problematic third molars in young adults is more often the case. -
Overcrowded Teeth
A tooth size to jaw size discrepancy often results in a crowded and misaligned smile. More simply put, the upper and lower jaws are not large enough to accommodate all the permanent teeth. As part of an orthodontic treatment plan to optimally align teeth and establish an attractive, healthy, and functional bite, the extraction of select permanent teeth may be required.
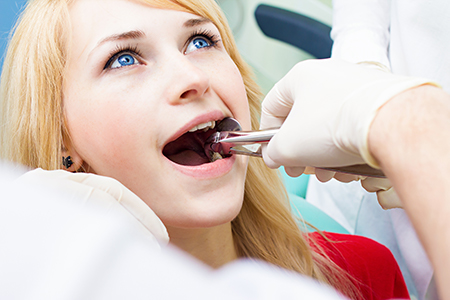
How is a tooth extraction performed?
Whatever the reasons for a dental extraction may be, you can rest assured that your care is in the best of hands at our office. As the first step in care, our dentist will review your medical and dental histories and discuss any special considerations in care.
It's essential to inform our office of any existing medical conditions or medications you are currently taking. In some situations, extra precautions, including premedication with antibiotics, a change in medication, and a medical clearance may be required. Follow all our pre-surgical directives and let us know if you are sick or have developed other symptoms on the day of surgery.
Our goal is to reduce any anxiety and help ensure patient comfort whenever a tooth extraction is necessary. In advance of the procedure, we'll discuss any medical considerations or precautions and go over our pre-surgical instructions. We'll also discuss post-surgical recommendations, including whether replacing the extracted tooth or teeth is needed and the best options in care.
To thoroughly assess the tooth and the type of extraction required, we perform a comprehensive examination and take digital radiographs as indicated. Extractions are typically categorized as either "simple" or "surgical extractions."
What Is A Simple Extraction?
When the tooth is clearly visible in the mouth and the root anatomy is not extensively hooked, fused to the surrounding bone, or otherwise unusual, it usually falls into the category of a simple extraction. Once the tooth and the surrounding tissues get sufficiently numbed with a local anesthetic, our dentist will loosen any attached periodontal tissues and apply forceps to remove the tooth. As with all dental procedures, we do all we can to help ensure your comfort and relaxation throughout every step in care. For patients who are anxious about dental work or certain procedures, we can discuss additional options in dental sedation.
What Is A Surgical Extraction?
For teeth that are severely broken down, anklylosed, or impacted, a surgical extraction is often indicated. We may refer you to an oral and maxillofacial surgeon to perform this procedure. During a surgical extraction, a small incision in the soft tissues and localized, precise removal of overlying bone provides greater access to remove the tooth. As with all tooth extractions, patients are given a local anesthetic to completely numb the involved tooth and the surrounding tissues. Once again, additional options in dental sedation, pre-surgical considerations, and directives are thoroughly discussed and explained.
What To Do After Getting A Tooth Taken Out
As skilled and experienced providers of care, we recognize that every case is different and provide treatment that addresses the unique requirements of each patient. Depending on a patient's specific needs, we provide post-operative instructions, including special instructions, limitations on activities, medications, and follow-up care that support optimal recovery and healing. In some cases, post-op care may also include the involvement of a patient's physician. In general, and unless modified otherwise by our office, the following post-operative guidelines apply to simple extractions.
Post-Op Care Following An Extraction
-
Maintaining gauze pressure
Following your extraction, some gauze to bite down on will be placed over the extraction site. By biting down and maintaining pressure on the gauze as instructed, any active bleeding should stop. You may change the gauze pad after the first hour. Continue to bite down for another 45 minutes if heavy oozing continues. While it's normal for a little oozing to continue for 24 hours, contact our office if you are still experiencing profuse oozing or bleeding. -
Until the local anesthesia wears off
Until the local anesthetic has completely worn off, it's essential to protect yourself from unintentionally biting or injuring your lips, cheeks, gums, or tongue. -
Take medications as prescribed
-
Antibiotics:
If you have been given a prescription for antibiotics, be sure to take the correct dosage and full course of medication as prescribed. -
Pain management:
It's helpful to take a pain reliever before the local anesthetic completely wears off. Over-the-counter (non-aspirin) pain medication may be taken to relieve discomfort. Any prescription pain medication should only be taken as directed.
-
-
To facilitate healing
Do not rinse your mouth, spit, drink through a straw, or suck on candies. It's essential to allow the extraction site to clot and not dislodge the new clot once it has formed. -
Applying ice
An ice-pack held in place in the facial area overlying the extraction site helps to control swelling. Apply the ice for 10-minute intervals during the first day following your procedure. -
Avoid smoking
Smoking not only prevents clot formation, but it also interferes with healing. Avoid smoking and tobacco products for the first week. -
Watch what you eat and drink
Stay away from hot or spicy foods and drinks for the first day or two. Also, refrain from drinking any carbonated or alcoholic beverages. Stick with a diet of soft foods and liquids for the first couple of days following surgery. Drink plenty of fluids. -
Oral hygiene
Brush gently; it's essential to take great care not to disturb or irritate the extraction site for a few days. A very mild lukewarm saltwater solution can be used to freshen your mouth. Remember not to rinse or spit that first day or two. Simply let any liquids gently fall from your mouth into the sink. -
An appointment for a follow-up visit
If sutures (stitches) were placed, or if a complex extraction, an infection, or other issues requires a visit to monitor your healing and progress, you will be given an appointment for follow-up care. It's essential that you keep this appointment as provided.
If you experience continued bleeding, ongoing pain, more swelling, have a bad taste in your mouth, or other unusual symptoms, contact our office.
Why choose the office of Hawthorn Dental Associates?
You deserve quality care that's personalized to meet your individual needs, and at the office of Hawthorn Dental Associates, you can rest assured your smile is in the best of hands. We deliver precise and gentle care, keeping you informed and relaxed throughout your procedure. If your tooth needs to be replaced, we'll discuss your best options, including dentures, fixed bridges, and dental implants. As the most advanced method of tooth replacement available, dental implants come the closest to replicating the look, feel, and function of a natural smile.
Dental Extraction FAQs
+What are the most common reasons for an extraction?
The most common reasons for tooth loss include advanced periodontal disease, extensive tooth decay, and facial trauma. According to statistics, gum disease is responsible for close to 70% of tooth loss in adults. Although less frequent than the preceding three reasons, it should also be noted that specific diseases, drugs, smoking, and poor nutrition contribute to the risk of tooth loss.
+How common is tooth loss?
The Centers for Disease Control and Prevention report that in the United States, an average of 12 teeth (including the wisdom teeth) are lost by the age of 50. Also, 26% of adults between 65 and 74 years of age have lost all their teeth.
+Does it hurt to have a tooth extracted?
Every patient and every situation is different. However, when a tooth and the surrounding tissues are numbed with a local anesthetic, you should only expect to feel a bit of pressure, but no pain as the tooth is being loosened from the surrounding tissues and extracted. For patients who are apprehensive and for some surgical extractions, our office will discuss our options in dental sedation to provide further relaxation and reduce any sense of discomfort.
+What will I feel when the anesthetic wears off?
While it's normal to feel some tenderness and swelling following an extraction, the degree of these sensations can vary. It mostly depends on the complexity of the extraction and the body's response to the procedure. We'll recommend or prescribe the appropriate pain medication to help ensure your comfort and give you specific instructions for maximum effectiveness and safety.
+How long does it take to recover from a tooth extraction?
Typically, the recovery period following a simple extraction is shorter than a surgical extraction. However, a patient's overall health, habits, and the size and location of the tooth, and other variables can influence recovery and healing. To speed up the recovery and avoid any complications, patients must follow the given at-home instructions diligently. We'll carefully review what to expect following your procedure and go over your post-op instructions.
+Why should one refrain from smoking following a tooth extraction?
Smoking interferes with blood clot formation, which is an essential first step in the healing process. Blot clot formation not only provides a protective layer to cover the underlying exposed bone and nerve endings, but it also supports the growth of new tissue. Cigarette smoke also contains chemical toxins that can disrupt the healing process and lead to problems such as continued inflammation, infection, or dry socket.
+What is dry socket?
In a very small percentage of cases, a condition known as dry socket can develop in the aftermath of a dental extraction. This painful condition can arise when the blood clot in the extraction site doesn't form properly or gets dislodged. With dry socket, you may experience throbbing pain and symptoms such as bad breath and an unpleasant taste in your mouth. As skilled providers of care, our office will provide immediate treatment to alleviate your discomfort and promote healing.
+Will I need my wisdom teeth extracted?
The last teeth in your mouth to develop, wisdom teeth often do not have enough room to fully erupt or may be positioned in the wrong direction. These issues can affect your dental health as well as overall wellbeing. While some individuals never develop all their wisdom teeth, and a few have sufficient space for them, there are many people with partially or fully impacted third molars. Our office will monitor the development, position, and health of your wisdom teeth and will advise you if and when extractions are indicated.
+What is the reason for a bone graft immediately following an extraction procedure?
After a tooth is removed, bone-grafting material is sometimes placed in the socket to promote healing and encourage new bone development. This procedure is often performed to support the eventual and successful placement of a dental implant.
+How much does getting a tooth taken out cost?
At the office of Hawthorn Dental Associates, we strive to make dental care affordable and accessible. Depending on the type or complexity of the extraction and other variables, the cost of the procedure can vary. Based on our diagnostic findings, our office will inform you of the healthiest choices in care, explain the fees, discuss insurance coverage, and explain your payment options.
+Are tooth extractions covered by dental insurance?
Many dental plans offer some level of coverage for tooth extractions. We'll advise you if your plan covers the full cost of the procedure and if there is any out-of-pocket expense. Our business office will work with you to maximize your insurance benefits as much as possible while helping you minimize any out-of-pocket expenses.
Replacing Missing Teeth With Dental Implants
If you're missing teeth, you're not alone. Tooth loss is a far more common problem than you think. In fact, studies show that 178 million people across the United States are missing at least one tooth, and 35 million are completely edentulous (missing all their teeth). Whether you have lost one tooth or multiple ones to gum disease, tooth decay, or a traumatic injury, the office of Hawthorn Dental Associates can help. We provide state-of-the-art care and offer the latest solutions to help patients reestablish complete, healthy, and beautiful smiles.
Dental implants for a smile that looks and feels completely natural!
Today, dental implants represent the most advanced system for the replacement of missing teeth. While conventional fixed bridges and dentures remain effective and satisfying ways to replace missing teeth, dental implants come the closest to replicating the look, feel, and function of a natural smile.
With dental implants, you can once again enjoy all your favorite foods and speak and smile with renewed confidence and ease. Because dental implants behave in much the same way as the roots of natural teeth, they provide unrivaled stability for the placement of a broad range of dental prostheses, including crowns and bridges up to a complete set of teeth. For patients who wear full dentures, dental implants provide the added stability and retention required to improve comfort and fit while preventing any embarrassing slippage.
If you are struggling with tooth loss and looking for the best solutions for the replacement of missing teeth, visit the office of Hawthorn Dental Associates to learn more about dental implants and all the state-of-the-art services we provide. At the office of Hawthorn Dental Associates, we take pride in creating beautiful and healthy smiles!

Let The Office Of Hawthorn Dental Associates Help You Rebuild A Beautiful Smile
Missing teeth do more than cause embarrassing gaps in your smile. For one thing, they can also affect your ability to speak or chew nutritious food with ease. By not replacing missing teeth, the adjacent ones can shift towards the space over time and change your bite and compromise the health of your smile in many ways.
With all of the advances in dental materials, technology, and treatment methods available today, it's easier than ever before to replace missing teeth with the most natural-looking and aesthetically pleasing results of care.
At the office of Hawthorn Dental Associates, we're pleased to offer leading solutions to improve your oral health and give you a smile you can feel confident sharing with the world. We give you back the complete smile you have lost and provide personalized solutions for all of your oral healthcare needs. To find out more about dental implants or schedule an appointment so that we can take a closer look at your smile, give us a call today.
Frequently Asked Questions
+What are dental implants?
Dental implants are small, biocompatible surgical posts that behave in much the same way as the roots of natural teeth. Once placed and integrated with the surrounding bone, dental implants provide unparalleled support for single crowns, bridges, and dentures. As the most advanced method for the replacement of missing teeth, they offer satisfying, long-lasting, and functional solutions for rebuilding a complete smile.
+What are the benefits of getting dental implants?
Whether you're missing one tooth, multiple ones, or missing all your teeth, you can rebuild a complete and beautiful smile with dental implants! According to statistics, roughly 3 million people have already received dental implants, with that number increasing at a staggering rate of 500,000 per year! The soaring popularity of dental implants is attributed, in large part, to the numerous benefits they offer as compared with other methods of care.
While conventional fixed bridges and dentures provide effective and satisfying solutions for the replacement of missing teeth, dental implants offer several advantages over traditional methods of care:
-
Dental implants come the closest to replicating the look, feel, and function of natural teeth.
-
With precise placement, good oral hygiene, and routine care, dental implants can last for many years.
-
Dental implants provide continued stimulation to the underlying bone to prevent the bone loss that occurs when teeth are missing while preserving natural facial contours.
-
Since implants behave like natural teeth, there is no chance that they will slip or dislodge like removable dentures when speaking or eating.
-
With dental implants, it is possible to speak with ease as well as eat and taste all types of food with virtually no restrictions.
-
Dental implants do not decay and will not develop cavities.
-
Unlike a fixed bridge, dental implants do not require any preparation or crowning of teeth adjacent to the edentulous area.
+Are dental implants right for me?
If you are wondering if you're a candidate for dental implants, it's easy enough to find out. At the office of Hawthorn Dental Associates, we're not only happy to take a look at your smile, but we'll also answer all your questions and explain your best options in care. As the most versatile solution for reestablishing a complete smile, dental implants offer a wide range of applications and can be used to replace a single tooth, multiple teeth, or all of the upper and lower teeth.
Rest assured that your care is in skilled and capable hands. You can count on our office for the best solutions for your smile. We treat every smile as unique and develop personalized treatment plans based upon your medical and dental histories, as well as your current oral health, cosmetic expectations of care, lifestyle, and budget.
+How are dental implants placed?
It's essential to plan and meticulously execute every step in care, from initial treatment planning and the precise placement of dental implants all the way to the design, fabrication, and insertion of the final crowns, bridges, or dentures.
Surgery to place the dental implants is typically considered a minor surgical procedure and performed on an outpatient basis. However, the exact extent of the procedure depends upon the type and number of dental implants and whether or not any additional procedures are required to prepare the supporting bone.
As your trusted partner in care, you can count on our office to keep you well informed every step of the way. Patient care and comfort are our top priorities. We do everything we can to put you at ease and make every visit to our office both comfortable and stress-free. Prior to your dental implant procedure, we'll discuss your dental anesthesia, options in dental sedation, and provide detailed pre-op and post-op care instructions.
Once your dental implant is placed, it can take a few months for it to fully integrate with the surrounding bone. While in some cases, a same-day temporary crown or bridge can be placed to provide an immediate and cosmetically pleasing look, permanent prostheses are typically placed when healing and osseointegration (fusion) with the surrounding bone are completed.
+Why might I need a bone graft to get a dental implant?
According to clinical studies, dental implants have a demonstrated long-term success rate of well over 95%. However, the long-term stability and success of a dental implant depend upon the presence of sufficient bone at the time of placement. In cases of periodontal disease or following the extraction of a tooth, bone volume is often lost. By placing a bone graft in the extraction site, or prior to the placement of a dental implant, we can establish sufficient bone support for a sturdy and stable dental implant.
+How much do dental implants cost?
While rebuilding a complete smile with dental implants is a worthwhile investment, our office is sensitive to the costs involved in dental care. We customize care and will discuss all treatment options that address your oral healthcare needs, cosmetic goals, and budget. Our office is dedicated to making care more accessible and will help patients navigate their dental insurance coverage and optimize their benefits. We can also discuss payment plans as well as financing treatment to make things easier for you. Feel free to contact our team with all your questions regarding methods of payment and financing options.
8 More Questions To Ask Your Dentist About Dental Implants
+Why is it so important to replace missing teeth?
Even if you've lost a back tooth that no one sees, it's essential to replace it. Missing teeth do more than cause embarrassing gaps in your smile. In addition to affecting your ability to chew and speak, missing teeth can also cause gradual changes to the alignment of your remaining teeth. These changes not only affect your bite, but they have the potential to create more unsightly and unhealthy gaps in your smile. Furthermore, without the support of a complete set of teeth, facial contours can begin to sag, creating a more haggard look over time.
+Are dental implants suitable if I am missing more than one tooth?
In addition to representing the most advanced solution for the replacement of missing teeth, dental implants are also the most versatile. While an individual implant supports a crown to replace a single tooth, additional implants can also be placed to replace multiple teeth. Even if you're missing all your upper or lower teeth, dental implants can be used to reestablish a complete and beautiful smile.
+How can dental implants help if I already wear full dentures?
Dental implants can help people who wear full dentures in multiple ways. For one thing, dental implants offer an alternative to full dentures. Because strategically placed dental implants can support a full arch dental bridge, you can enjoy the benefits of a fixed, non-removable, stable, and natural-looking solution for your smile.
Another way dental implants can benefit someone who wears full dentures, is by providing the denture with added stability and retention. Specialized dental implants offer an attachment point for a full denture so that you no longer need denture adhesives to prevent uncomfortable and embarrassing slippage.
+Are dental implants safe?
Just like a new hip or new knee, dental implants are fabricated from the highest quality of medical-grade biocompatible materials. While most dental implants are made of titanium, some are fabricated from zirconia. Both titanium and zirconia are biocompatible materials, which integrate well with the hard and soft tissues in the jaw.
+Will dental implants give me a natural-looking smile?
Dental implants behave in much the same way as the roots of natural teeth and are designed to support both individual dental crowns and bridges to rebuild a complete smile. Just how aesthetically pleasing and naturally beautiful your dental implant restorations look depends in large part on the artistry and skill of the professionals providing your care.
At the office of Hawthorn Dental Associates, you can feel confident sharing your new smile with the world. Every implant restoration that we fabricate is made from the most cosmetically pleasing, safe, and durable dental materials. Not only will your new teeth blend seamlessly with your smile, but the size, shape, and color will be selected for optimal facial aesthetics and harmony.
+How do I take care of my dental implants?
Taking care of your dental implants requires the same diligence it takes to care for a natural smile. An effective oral hygiene regimen that includes brushing twice a day and flossing combined with healthy oral habits, good nutrition, and routine dental care are the best steps you can take to maintain your new smile. Although dental implants do not get cavities, it's essential to keep in mind that you can still develop periodontal problems, compromising the success and longevity of your dental implants.
As your trusted partner in care, we remain dedicated to your ongoing oral health. We'll provide you with ample instruction in the best methods for taking care of your oral health and new smile.
+How long do dental implants last?
Dental implants enjoy the highest success rate of any implanted medical prosthesis. However, their longevity depends on a number of factors. Enjoying the benefits of dental implants in the long term relies upon skilled placement, adequate bone volume at the time of placement, and the level of ongoing oral care. With proper care, well-planned and well-placed dental implants will serve you well for many years to come.
+Why choose the office of Hawthorn Dental Associates?
As skilled and experienced providers of care, our office values patient input, and a member of our team is always on hand to address all your questions and concerns. We firmly believe that achieving the best treatment outcomes depends upon successful partnerships in care. We strive to provide the best solutions for your smile while making treatment more comfortable, accessible, and affordable. We tailor care and meticulously treatment plan cases to address the unique requirements of every smile. With dental implants from our office, you can once again enjoy all your favorite foods and feel more confident in all your social and professional interactions.
If you are interested in hearing more about dental implants and whether they offer the right solution for your smile, give us a call today. We're happy to explain all your options in care.
An innovative, discreet, and effective system of care, Invisalign® treatment offers a cosmetic way to align your smile with minimal interference to daily activities using a series of clear aligners.
With aligners that are practically invisible, only you will know that you're undergoing orthodontic care! Invisalign may, in most cases, eliminate the need for unsightly, uncomfortable, unattractive bands and wires. Whether you are a teenager who needs braces to correct a malocclusion or an adult who would like to straighten out some crooked teeth, Invisalign may well be the answer for you!
Invisalign utilizes 3-D computer imaging technology to correct problematic bites or malocclusions by planning a complete sequence of custom-made clear aligners. This series of clear aligners incrementally move the teeth into place until the final desired corrections are reached.
With Invisalign® clear aligners, your treatment is tailored to you. Innovative technology combines with a personalized treatment plan to make custom clear aligners for creating your new smile.
As pioneers in the field of aligner development and technology, the folks at Align Technology, Inc. gather data from millions of treated smiles to design treatment systems that:
- Are faster, more advanced and comfortable than other options in care.
- Are able to address a broad spectrum of malocclusions ("bad bites") and teeth alignment issues.
- Allow more precise planning and control of multiple types of tooth movement.
Custom-made to the exact specifications of your smile, Invisalign clear aligners are designed to incrementally move your teeth into their correct positions over time. Simply swap-out last week's aligner for the next one in the series and watch as your smile progressively shows signs of improvement.
And, because Invisalign clear aligners are removable for short periods of time, as opposed to traditional braces, you can still enjoy the foods you love as well as brush and floss your teeth with ease!
Whether you are a teen who needs braces or an adult who yearns to "fix" their smile, Invisalign clear aligners may be the perfect solution for you! Contact our office for more information and to schedule a consultation for care.

Come in for a consultation
Your doctor will examine your teeth and show you what Invisalign treatment can do for you.
Get your personalized treatment plan
Start with a fast, precise digital scan. Then your doctor will map out a custom treatment plan just for you. You will even get a preview of your smile.

Your aligners are customized for you
Your clear aligners are created using industry leading technology based on your customized treatment. Your aligners are created with comfort in mind.

Pick up your first aligners
From the first day of treatment to the last, you're never on your own — your doctor will be with you every step of your way.
The difference is clear
Explore the true stories and journeys of several Invisalign patients
*Invisalign is a registered trademark of Align Technology, Inc.
Frequently Asked Questions
+I want to straighten my teeth but I don't want metal braces. What are the alternatives?
There are many options for patients who want to avoid metal braces! The most popular alternative orthodontic treatment is Invisalign®, which are clear plastic aligners designed to straighten teeth. After an examination of your teeth, your dentist will determine which option is best suited to your wants and needs.
+Is Invisalign® expensive?
According to the Invisalign® website, the cost for treatment is approximately the same as the cost for metal braces. A portion of this cost may be covered by your insurance. Please call Hawthorn Dental Associates to set up a consultation and discuss potential payment plan options.
+How does Invisalign® work?
The first step is to schedule a consultation with your doctor, so they can devise a treatment plan that is best suited to your individual dental needs. Once approved, you will receive your first set of aligners. Your doctor will then regularly monitor the movement of your teeth and new aligners will be ordered according to the progress made in your treatment plan.
+What is Invisalign® made of?
Invisalign® aligners are made of clear, flexible plastic. The company received a patent for this material – SmartTrack® – to be used exclusively for Invisalign treatment purposes. These aligners are FDA approved and nearly invisible!
+How long does Invisalign® treatment take?
Your doctor will give you an estimate regarding how long your Invisalign® treatment should take, which will depend on your specific needs. The average length of time for treatment is approximately 12-18 months. However, some patients may see results far sooner. Remember to wear your aligners exactly as instructed by your doctor to obtain the best results.
+Are Invisalign® results permanent?
Your doctor will most likely recommend that you wear retainers following your Invisalign® treatment. This is a precaution that will prevent your teeth from shifting back to their original positioning. It is important to follow your doctor's instructions exactly to ensure long-lasting results.
+How often must I wear my aligners?
You must wear your aligners for up to 22 hours daily. You may remove them for eating, drinking and regular oral hygiene.
+Are there any restrictions to what I can eat while in treatment?
No. Unlike braces, you may eat whatever you like as long as you remove the aligners before eating. Prior to placing the aligners back on, it is important to brush your teeth and the aligners after you eat.
+Will wearing the aligners affect my speech?
Like any orthodontic treatment, there is a short adjustment period. The more you speak with the aligners on, the quicker you will adjust.
+Is there any discomfort with Invisalign® treatment?
There will be some pressure and minor discomfort for a day or two after each initial insertion. This is a sign that your teeth are moving sequentially into their final position.
+Can I chew gum?
It is recommended that you remove your aligners prior to chewing gum as the gum will stick to the aligners.
+Can I smoke with the aligners in?
We discourage smoking with aligners as the cigarette smoke will tend to discolor them.
+How do I keep my aligners clean?
Brushing them with toothpaste will keep them fresh and clean.
+How often do I see an orthodontist while wearing Invisalign®?
Regular office visits are every five to six weeks. This will ensure that your Invisalign treatment is progressing as planned.
+What happens after my treatment is complete? Do I need retainers?
All orthodontic patients are instructed to wear their retainers at night indefinitely. Sleeping with your retainers in at night will ensure a healthy bite and maintain the new position of your teeth.
+How long does Invisalign treatment take?
Treatment time varies depending on the severity of the misaligned teeth. Treatment time can be shorter than traditional braces, between six and 18 months.
+Does Invisalign work for kids?
Yes, if their teeth, including second molars, have grown in completely.
Oral cancer accounts for 2.9% of all diagnosed cases of cancer in the United States. According to the American Cancer Society it is estimated that 51,000 people across the country will develop oral cancer this year and that 10,000 fatalities are expected from the disease.
Oral cancer can occur anywhere in the orofacial complex but is most often found on the tongue, the tonsils and oropharynx, the gums, floor of the mouth, lips, cheek lining or the hard palate. While the disease can affect anyone, men are twice as likely to develop oral cancer as women. Those particularly at risk for oral cancer are men over the age of 50 who are heavy smokers and frequently drink alcohol. Additional risk factors may include UV exposure from the sun or sunlamps, GERD (gastro-intestinal reflux disease, prior head and neck radiation treatment, exposure to certain chemicals and poor diet. While the death rate from oral cancer has been decreasing in the past several decades thanks to early detection and advanced methods of treatment improving the outcomes of care, there has been a recent rise in the incidence of oropharyngeal cancer due to increased transmission of the sexually transmitted human papillomavirus (HPV).
As part of a comprehensive exam, the dentist will perform a screening for oral cancer. To start, the dentist will review the patient’s medical and dental histories and ask if there have been any changes to his or her oral health or overall health. The dentist will then carefully check in and around the oral cavity as well as the head and neck area for any of the following signs or symptoms that may indicate the presence of a problem.
At the office of Hawthorn Dental Associates, the health and development of your child's smile are our top priorities. Our goals are to help children establish a strong foundation for a lifetime of good oral health and experience the benefits of healthy, beautiful smiles.
Excellent Oral Health Begins With Good Oral Care
All parents want what's best for their families. When good oral care, including routine dental checkups, start at an early age, our office can closely monitor the development and health of your child's smile as they grow. It's essential to keep in mind that preventive care and timely treatment for any emerging dental issues not only helps to ensure ongoing oral health but also supports overall well-being, and contributes to a positive self-image.
You can rest assured that your child's smile is in the best of hands at our office! We provide gentle and precise care in an environment that's comfortable, warm, and engaging. At the office of Hawthorn Dental Associates, we offer a comprehensive range of dental services designed to address the dental needs of children of all ages. Whether it's your little one's first trip to the dentist, a routine visit, treatment for a dental emergency, or more, we're well equipped to provide the care that's needed.
We take a proactive approach and emphasize the importance of dental prevention as the key to good oral health. We provide you and your child with the resources as well as the tools to establish an effective brushing and flossing routine and offer nutritional guidance and advice on potentially harmful oral habits. Our entire team strives to make each visit with your child a positive, informative, and beneficial experience.

The Importance Of Regular Checkups And Routine Care
Studies show that children and teens lose an estimated 51 million school hours each year to dental problems. To help your child maintain optimal oral health and a smile that's healthy and bright, we recommend dental checkups and cleanings twice a year.
As skilled and compassionate providers of care, we understand all aspects of dental development and are sensitive to the unique needs of children. At each periodic exam, a member of our professional team will review your child's medical and dental history and then perform a thorough clinical assessment of the teeth, gums, jaws, and the surrounding oral tissues. We'll also check your child's bite, jaw alignment, and function.
Because it's vital to see what's going on below the surface, we'll take digital radiographs as needed, to check for the presence of any cavities, or infection and to evaluate the position of your child's developing teeth and the health of jaw bone. We'll also perform a professional dental cleaning to eliminate any plaque or debris that has accumulated between the teeth or in hard to reach places.
Tooth Decay Is The Single Most Common Chronic Childhood Disease
At every stage of your child's development, we'll advise you on the most effective methods of keeping his or her teeth clean and discuss the foods, beverages, and harmful oral habits that can lead to problems. While it can be difficult sometimes to get children into a regular oral hygiene routine, we'll give you tips and advice on how to make brushing and flossing a fun part of their daily activities. As your trusted partner you can rely on the office of Hawthorn Dental Associates to keep a close watch on your child's oral health and development.
By following these simple guidelines, you can help your child maintain optimal oral health and develop a positive attitude towards dental care:
-
Establishing a dental partnership when your child is small
-
Keeping your baby's and toddler's teeth clean
-
Not allowing your baby to sleep with a bottle of milk or juice.
-
Bringing your child to the dentist for routine checkups and care
-
Leading by example and encouraging the recommended tooth brushing and flossing routine
-
Promoting wise dietary choices and healthy snacking, including replacing sugary drinks with water and limiting sweets
-
Providing supportive guidance to help your child put away their pacifier and stop thumb or finger sucking at the appropriate time
-
Making sure your child wears a mouthguard when playing specific sports

Your Baby's Smile
Even before your child is born, your little one's first set of teeth is already forming. As a matter of fact, by the time your baby is a year old, some of the front teeth will have already emerged into place. For this reason, it's essential to establish an oral care routine at an early age. As per the recommendations of the American Dental Association and the American Academy of Pediatric Dentistry, parents are encouraged to have their baby see the dentist around the time of their first birthday.

More On Dental Care For Children and Teens
Childhood is a time of incredible physical and emotional changes. As kids go through several stages of development, so do their teeth. Many things, including both genetic and environmental factors, contribute to the health and appearance of your child's smile. While some issues cannot be prevented, there's still a lot you can do to help ensure your child experiences optimal oral health and develops an attractive, functional smile. Our office will make sure your children are instructed in the best methods for caring for their teeth and will provide them with useful, age-appropriate information on following a healthy diet as well as make them aware of which oral habits and activities may be harmful to their teeth and overall well being.
Assessing Facial Growth And Dental Development
In addition to checking for the presence of dental disease, we also monitor your child's facial growth, jaw development, and alignment of their smile. If orthodontic treatment is indicated, we'll advise you of our recommendations for care. Since many children and teens wear braces, paying extra attention to what they eat and how they maintain their oral hygiene is of the utmost importance.
Good nutrition is essential for a healthy smile
Beyond good oral hygiene and routine dental care, a balanced, nutritious diet is essential for a healthy smile in a growing child. Sticky, sugary foods and drinks are not only harmful to children's oral health but also detrimental to their overall well-being. A diet rich in nutrients is critical for optimal growth and development and keeping the teeth and gums strong.
FAQs On The Topic Of Your Baby's Smile
+When will my baby's first tooth appear?
A baby's first teeth begin to appear in the 6 to 12-month range. Typically, it's the two lower front ones that appear first. The baby teeth come into place from the front of the mouth and then on to the back. With that said, most children will get all of their baby teeth by the time they are three.
+How should I clean my baby's new teeth?
For babies with new teeth just emerging, we may recommend just a washcloth or infant toothbrush to start. As your baby grows and more teeth come into place, an age-appropriate soft bristled brush, and a tiny dab of toothpaste will be recommended. One word of caution; be careful that your child does not swallow the dab of toothpaste. When your child gets older, we will teach him or her more about the responsibilities of self-care and oral hygiene.
+What should I do if my baby is teething?
While getting teeth is an important milestone in a baby's development, it's essential to be aware that teething can make a baby quite irritable. Your little one may act fussy, have trouble sleeping, avoid eating, and drool quite a bit. While you are powerless to speed up the process of teething, there are a few things that you can do to soothe your baby as their new teeth are erupting into place. Common approaches to helping your baby feel more comfortable while getting their new teeth include safe teething rings, a cold spoon, or a moist gauze rubbed over their gums. Remember, you can always call our office if you have any concerns.
+Why are baby teeth so important?
The first set of teeth not only makes it possible for your baby to smile, eat, and speak, but they also play the critical role of serving as placeholders for the permanent teeth. Losing a baby tooth too early can potentially result in a misaligned smile.
+Can babies develop tooth decay?
When caring for your child's smile, it's important to remember that baby teeth are just as susceptible as the permanent teeth to decay. In fact, more than 50% of children develop cavities before the age of five. Not only does tooth decay pose a risk to the health of the involved baby teeth, but untreated cavities can also have consequences for your child's overall well-being and the permanent teeth that are yet to come into place.
+What is baby bottle syndrome?
Baby bottle syndrome, which is also known as nursing bottle syndrome, refers to the rampant tooth decay that results from babies sleeping with a bottle containing milk or juice. While the damage is most prevalent in the front teeth of the upper jaw, extensive dental work is typically required to restore the toddler's oral health and prevent infections. New parents are advised not to let their baby sleep with a bottle or at least swap the juice or milk for water.
+Will thumb or finger sucking affect the development of my child's smile?
Some children persist in sucking their thumbs or fingers beyond their preschool years. For these children, the activity continues to be a source of comfort, relaxation, and security. It may even help them fall asleep at night. However, it's essential to be aware that in the long-term, a finger sucking habit is not healthy.
If your child is still thumb or finger sucking by the age of five or six years, it's time to constructively help them stop the habit. If it has caused any alterations to the alignment of the teeth or jaws, or if it is affecting your child's speech or swallowing patterns, it's likely your child requires orthodontic care.
FAQs As Your Child Grows
+How often should my child have a dental checkup?
The American Dental Association advises parents to bring their kids in for a routine checkup and preventive care once every six months. At this time, our dentist will examine the teeth, gums, and jaws to assess your child's overall dental health and development. Your child will also have a dental cleaning performed in addition to receiving age-appropriate oral hygiene instructions and nutritional guidance. If any emerging issues are detected, our office will provide the treatment required to address these problems early in their onset.
+What if my child is anxious and has difficulty sitting for treatment?
At the office of Hawthorn Dental Associates, we take pride in providing gentle, compassionate care in an environment that is designed with comfort in mind. However, every child is different. While for some children, a trip to the dentist is taken in stride; for others, it can present challenges and produce significant anxiety. If your child is apprehensive, has a medical condition, special needs, or difficulty sitting in a dental chair, we can discuss the best choices for the provision of care and options in dental sedation.
+Why are back-to-school checkups so important?
Helping your child start the school year on the right foot not only means getting the correct school supplies, but it also involves making sure your child is in the best of health. One key to avoiding setbacks during the academic year is to make sure your child's smile is in tip-top shape! At the office of Hawthorn Dental Associates, we specialize in addressing the dental needs of children as well as helping them establish a strong foundation for a lifetime of optimal oral health.
+What causes cavities?
Cavities develop when plaque is not consistently removed from around the teeth and gums. Due to inadequate oral hygiene practices and dietary habits, children are especially prone to developing cavities. As an added level of protection against tooth decay in children, our office typically recommends periodic fluoride treatments and dental sealants.
+What is a space maintainer?
Sometimes, due to tooth decay or a traumatic injury, a child may lose a primary tooth early, before the permanent one underneath is ready to come into place. When this happens, our dentist will consider the best way to hold the space left by the baby tooth in order to maintain a clear path for the succeeding adult tooth. Sometimes a small dental appliance, known as a space maintainer, is required to make sure the permanent tooth does not become crowded out of the dental arch or impacted by shifting adjacent teeth.
+When is the best time to begin orthodontic care?
In addition to checking for the presence of dental disease, harmful oral habits, as well as the presence of other unhealthy activities or conditions, our office will also monitor your child's facial growth, jaw development, and alignment of their smile. If orthodontic treatment is indicated, we'll advise you of our recommendations for care. One common misconception regarding orthodontic treatment is to wait until all of the permanent teeth (except the wisdom teeth) are present. However, most problems involving the alignment of the teeth and jaw growth can be identified by the time a child is in the first or second grade. For this reason, the American Association of Orthodontists recommends that all children have a check up with an orthodontic specialist no later than age 7.
+What's the best way to protect a child's smile if they play sports?
If your child or teen plays sports, a sports mouthguard is an excellent idea. Properly fitted, mouthguards are a fundamental component of protective athletic gear and have been demonstrated to reduce trauma to the teeth, tongue, lips, and jaws. Based on your child's involvement in a particular sport, we'll advise you on the most appropriate mouthguard to protect his or her smile.
+Why are dental sealants recommended?
After your child's permanent molars and premolars come into place, we typically recommend the placement of dental sealants. As an ultra-thin, clear coating that is painlessly applied to the biting surfaces and grooves on the back teeth, dental sealants block the bacteria and acids that cause decay.
+Will my child's wisdom teeth require extraction?
Wisdom teeth, which are also known as the third molars, are the last permanent teeth to develop in the oral cavity as well as the final ones to come into place. However, as is often the case, many wisdom teeth do not have sufficient room to erupt, are not developing correctly, or are causing issues for the adjacent teeth and the surrounding tissues. If the wisdom teeth are not fully or partially impacted, they tend to emerge between the ages of 17 and 21 years. At every checkup visit, our office will monitor the development and position of your child's wisdom teeth recommend if and when any extractions are indicated.
+What if my child has a dental emergency?
Recognizing the fact that children have active lifestyles means there is always a chance an accident involving a hit or blow to the mouth or teeth can occur. These traumatic injuries can happen at home, in the playground, or on the playing field. Common injuries to the teeth and oral cavity seen in a pediatric dental office include everything from soft tissue lacerations of the lips, cheeks, or tongue to chipped, fractured, dislodged, or "knocked out" teeth.
Equally frequent reasons for children to require urgent dental care are painful toothaches, dental infections, and mouth ulcerations. Whatever your child's dental emergency may be, you can rely on our office to provide skilled, compassionate, and reliable care. Our goal is to get your child back on the road to oral health while alleviating any associated discomfort and preventing more serious consequences to their dental health and overall well-being.
+Why choose the office of Hawthorn Dental Associates
At the office of Hawthorn Dental Associates, we welcome patients of all ages for care and provide a comprehensive range of services designed to address the needs of every member of your family. We're passionate about what we do and maintain a position at the forefront of advances in dentistry to offer our patients the best options in care. You can depend on our office to help you and your children enjoy good oral health. To schedule an appointment, or to learn more about our office, give us a call today.
Did you know that the most common cause of tooth loss in adults is gum disease? According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease. However, the good news is that periodontal disease is almost entirely preventable. At the office of Hawthorn Dental Associates, we offer a comprehensive range of services to help patients maintain optimal periodontal health and enjoy the benefits of a smile that look, feels, and functions at its best.
What is periodontal disease?
Periodontal disease, more commonly known as gum disease, is a set of inflammatory diseases that affect the "periodontium", which are the hard and soft tissues surrounding and supporting your teeth. Just like tooth decay, gum disease is attributed to the harmful bacteria in dental plaque and tartar that accumulate around the teeth and under the gums.
Since the progression of periodontal disease is often painless, you may not even be aware of an ongoing disease process. For this very reason, it’s essential to practice good oral hygiene and schedule visits for regular checkups, professional cleanings, and routine care.
Taking care of your smile includes being mindful of the signs and symptoms of gum disease.
Some indications that you may have periodontal disease include:
-
Inflamed and red gums
-
Bleeding when brushing or flossing
-
Receding gums and exposed tooth root surfaces
-
Sensitivity to hot or cold temperatures
-
Bad breath or a bad taste in the mouth
-
Teeth that feel loose
-
New spaces developing between the teeth or a change in the bite
-
Change in the fit of existing partial dentures
-
Discharge around the teeth and gums
-
Sharp or dull pain when biting down or chewing food

The Importance Of Good Oral Health
Taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, and respiratory problems.
At the office of Hawthorn Dental Associates, we emphasize the importance of prevention, early detection, and timely treatment of periodontal disease. We provide patients the guidance, support, and care required to maintain optimal periodontal health.
What is gingivitis?
Gingivitis represents the initial stage of gum disease. Although it doesn’t cause overt discomfort and often goes unnoticed, there are specific signs to be aware of that indicate the start of a problem. If you notice your gums bleed when you brush, look red and inflamed, or feel a little tender, you more than likely have gingivitis.
The good news is that by treating gingivitis early, the tissue damage associated with more advanced stages of gum disease can be avoided. Despite the presence of inflammation, the overall integrity of the periodontal tissues in this stage remains intact.
Treatment instituted at this point is often sufficient to reverse the course of the disease and to avoid any permanent damage to the periodontal tissues. A series of deep dental cleanings, an improved home care regimen and a commitment to regular maintenance may be all that is required to prevent this stage of periodontal disease from progressing.

What is Periodontitis?
When left untreated, a case of gingivitis develops into a more advanced and damaging stage of gum disease, known as periodontitis. At this point, the connective tissue and bone that hold the teeth in place begin to break down. With the progression of periodontal disease and periodontitis, more and more tissue loss ensues. Damage often includes an increase in pocketing between the teeth and bone, gum recession, and bone loss. As unresolved periodontitis goes from mild to moderate to severe, it increasingly compromises the soft and hard tissues supporting the teeth.
Periodontal treatment in this phase is designed to halt the progression of the disease and to restore tooth support as possible. Treatment may involve medications to control the bacteria and reduce the size of the pockets between the teeth and gums, gum surgery, as well as bone and tissue grafts.
Let Us Help You Maintain Optimal Periodontal Health
At the office of Hawthorn Dental Associates, we offer personalized, state-of-the-art solutions to help you maintain healthy gums and an attractive, well-functioning smile. As skilled providers of care, we utilize leading-edge technology and treatment methods to address a broad range of periodontal conditions and needs.
Thanks to advances in care, periodontal treatment today not only helps to halt the progression of gum disease but also delivers effective solutions, including bone grafting and regenerative procedures to repair tissue damage, restore bone volume, improve cosmetics, or provide adequate support for the placement of dental implants.
How is gum disease treated?
The type of periodontal treatment you receive depends on several factors including the stage of periodontal disease, the extent of tissue damage, your overall oral health, existing medical conditions, and other considerations in care. After a thorough assessment of your case, we’ll discuss your options to reestablish and maintain optimal periodontal health. We welcome your questions and are always on hand to provide guidance and address your concerns.
Periodontal treatment can be categorized in the following ways:
-
Non-Surgical Periodontal Treatment
When periodontal disease is detected early in its onset, conservative or non-surgical methods of care combined with improved hygiene routines can restore periodontal health. While periodic, professional cleanings are sufficient to maintain periodontal health in patients that do not have gum disease, once gingivitis is present, deeper cleanings and possibly other non-surgical methods of care are recommended to treat the condition.
The American Academy of Periodontology emphasizes achieving periodontal health by means of the least invasive and cost-effective treatment approaches to care. Deeper cleanings, which include Scaling and Root planing, are non-surgical procedures that are considered the first line of defense against the progression of periodontal disease.
With scaling and root planing, any plaque and tartar (hardened dental plaque) that have accumulated below the gumline are carefully removed, and then the root surfaces of the teeth are smoothed. Since periodontal disease is an inflammatory response to plaque, tartar, and bacterial toxins, by simply mechanically eliminating these agents, the progression of gum disease can be halted. In addition to removing plaque and tartar with a scaling and root planing procedure, antimicrobial medication placed under the gumline or systemic medications can be used as adjuncts to care to further reduce the bacterial population.
If non-surgical approaches to managing periodontal disease do not achieve the desired outcome, surgery may be recommended to halt its progression and repair damage as possible.
-
Periodontal Surgery
When gum disease has advanced beyond the initial stage, periodontal surgery is often recommended to effectively remove bacteria and tartar from around the teeth, reduce gingival pocket depth, restore lost tissue as possible, and halt disease progression. It’s essential to keep in mind that gum disease is a progressive condition. If appropriate measures are not taken, gum disease continues to compromise the support of the teeth and have consequences to one’s overall dental health and well-being.
As untreated gingivitis evolves into more advanced stages of gum disease, periodontal pockets deepen, the bacteria become more difficult to remove, and the gaps between the surface of the teeth and gums get larger. When pocket depth increases to the point of being beyond the reach of deep cleanings and other conservative methods of care (5mm or more), gum surgery to clean and treat the damage to gums and underlying bone is typically recommended.
The good news is that with proper surgical treatment followed by improved oral hygiene, the chances of tooth loss, further damage to the bone and soft tissues supporting the teeth, and complications from health problems that are linked to periodontal disease can be decreased.
The goals of pocket reduction surgery are to accomplish the following:
-
Remove sub-gingival bacteria beneath the gums and from the surfaces of the roots of the teeth
-
Halt damage to the underlying bone, and recontour the affected hard tissues as needed
-
Reduce pocket depth to facilitate easier cleaning of the teeth and gums and the maintenance of optimal periodontal health
In many cases, a periodontal procedure, which is known as flap surgery, is frequently recommended. During this procedure, the gums in the affected area are reflected away from the teeth and supporting bone. Now, the pocket and roots of the teeth can be thoroughly cleaned and supporting tissues recontoured as needed. When this step gets completed, the tissue flag gets sutured back into place.
Today, in addition to conventional surgical approaches to care, dental lasers are also used to perform select periodontal procedures. When applicable, laser technology can help treat periodontitis, reduce pocket depth, address peri-implantitis, and remove or recontour gingival tissues for cosmetic purposes.
-
Gum Disease FAQs
+How common is gum disease?
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
+What causes gum disease?
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
+Are there other risk factors for periodontal disease?
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
+Why are healthy gums so important?
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
+What are the symptoms of gingivitis?
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
+What happens as gum disease progresses?
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
+What are the best ways to manage and treat more advanced gum disease or periodontitis?
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
+How much does periodontal treatment cost?
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
+What is the best way to prevent gum disease?
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
+Why choose the office of Hawthorn Dental Associates for care?
At the office of Hawthorn Dental Associates, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
For more information on our office and the many services we provide, give us a call today.
If you are told that a tooth requires a root canal procedure, there’s no need for alarm. Today, a root canal procedure is as routine and comfortable as receiving a dental filling. As a matter of fact, a root canal procedure is typically the best way to relieve toothache pain, save a damaged tooth, and preserve your natural smile.
At the office of Hawthorn Dental Associates, we use the latest technology to provide precise and gentle care to help patients maintain healthy, beautiful smiles. Patient care and comfort are our top priorities, and you can rest assured your oral health is in the best of hands.
An effective way to preserve your natural smile
With a demonstrated success rate of well over 90%, root canal procedures remain the most effective way of saving and retaining a tooth that has been severely compromised by dental decay or injury. Because having a healthy natural dentition supports your oral health and overall well-being, root canal therapy, as opposed to having the involved tooth extracted, is a routine and widely recommended procedure. Across the United States alone, root canal procedures are routinely performed almost 41,000 times daily and close to 15 million times per year.

Why you may need root canal therapy
Your teeth are much more than just the hard outer biting surfaces and the roots. Inside each one is a central chamber containing connective tissue, a nerve supply, and blood vessels. Collectively, these core tissues, known as the dental pulp, help your tooth to grow and mature before it emerges into the mouth. Once your tooth is in place, the dental pulp provides nourishment, keeps the tooth vital, and alerts you of problems.
Having sensitivity to various stimuli like biting down and eating or drinking hot or cold items is a warning from the nerves inside your tooth that dental decay is present, dental trauma has occurred, or infection is brewing. The degree of pain that you experience depends on the extent of the damage and nerve involvement.
When a tooth needs a root canal, it is because the dental pulp has become irreversibly damaged or has died. However, if enough intact tooth structure remains, and there’s good bone support around the compromised tooth, you do not need to have the tooth extracted. A fully developed tooth does not require the dental pulp to remain functional. You can preserve your natural tooth by having your dentist perform a root canal on the tooth.
Although not every instance of dental discomfort indicates the need for root canal therapy, some of the warning signs that you might require this procedure include the following:
-
Unresolved, persistent pain
Pain is your body’s way of signaling that something is amiss. Although, there are many explanations for oral pain, one of the most common reasons is a toothache caused by decay or damage that has affected the tooth’s inner vital tissues. Patients in need of root canal therapy often report dental pain that wakes them up at night.
-
Temperature sensitivity
If the pleasure of sipping hot beverages or foods are overshadowed by dental pain that makes you wince, it's time to contact our office. Extreme sensitivity to hot or cold foods and drinks can indicate an inflamed, irritated, or non-vital dental pulp.
-
Discomfort with pressure or the slightest touch
If it hurts when you bite and chew or when you just touch the tooth, it may indicate pulpal involvement, irreversible damage to the inner vital tissues of the tooth, or the presence of an infection.
-
Darkened, discolored tooth
A discolored tooth is often a message that the inner vital tissues, including the tooth’s nerve and blood supply, have been compromised. Teeth that have sustained an injury may demonstrate discoloration as the internal tissues have devitalized.
-
Chipped, cracked, or fractured tooth
An injury that chips or fractures a tooth can also traumatize the dental pulp or even compromise so much tooth structure that a root canal procedure is required to save the tooth.
-
Swelling around the tooth and gums
Swelling of the gums around a tooth may indicate that an infection has developed. While the swelling can worsen and cause more harmful consequences, sometimes a dental abscess starts to ooze pus and drain. In either case, prompt care is required.
-
Tooth mobility
The pathology associated with a tooth need of root canal therapy can damage the bone supporting the tooth and produce some mobility. Root canal therapy can often resolve this issue as tissue healing occurs.
The importance of timely care
While some of the above signs and symptoms can indicate other dental problems, they all require prompt evaluation and care. In some cases, a tooth in need of root canal therapy has not yet demonstrated overt symptoms. It may first get diagnosed and brought to your attention following a comprehensive, routine exam. Typically, these teeth show radiographic evidence of periapical pathology (root end pathology) or other types of structural damage.
It is essential that when a root canal is recommended that you receive timely care. Delaying the procedure increases the risk of more widespread and severe symptoms developing. A dental infection can pose significant consequences to your oral health and even threaten your overall health and well-being.
How is a root canal procedure performed?
With the modern dental instruments and advanced techniques available today, having a non-surgical root canal procedure is often as comfortable as getting a routine dental filling.
While some root canals can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on factors such as the number of canals in a tooth, its anatomy, and whether an active infection is present.
During a root canal procedure, our dentist will remove the diseased dental pulp, clean the internal portion of your tooth, and then fill all the prepared canals with a biocompatible filling material. Root canal therapy is typically performed under local anesthesia, but additional options in dental sedation are available to reduce any anxiety associated with dental procedures.
What to expect following root canal treatment
At the office of Hawthorn Dental Associates, the care and comfort of our patients are our top priorities. Our goal is to help our patients enjoy optimal oral health and to keep them well informed every step of the way.
After your root canal procedure, you may experience the following:
-
Until the anesthesia wears off
Immediately following your dental visit, you may experience a period of lingering numbness. Normal sensation typically returns within an hour or two. However, until the anesthetic has completely worn off, it’s essential to protect yourself from unintentionally biting or injuring your lips, cheeks, gums, or tongue. Be mindful of chewing, drinking hot beverages, or smoking.
-
Post-procedure discomfort
A root canal procedure will alleviate the pain of a toothache. However, you may still experience some mild to moderate discomfort in the immediate aftermath when the anesthesia wears off. These feelings should subside within days. To help prevent any undue pressure, which may cause pain, the biting surface of the involved may be slightly filed and taken out of occlusion. Our office will also recommend appropriate over-the-counter pain medications and provide a prescription if indicated.
-
Take any antibiotics as prescribed
If you have been given a prescription for antibiotics to treat or prevent an infection, it’s essential to complete the course of medications as prescribed.
-
Be mindful of the involved tooth
Even with a temporary filling, a tooth with a root canal remains vulnerable to stress and can fracture until a permanent crown or suitable permanent restoration is placed. In the interim, be mindful of the involved tooth. Try to chew on the opposite side of the mouth and avoid hard and sticky foods.
-
Continue to brush and floss
While you need to be mindful of a tooth that has received root canal therapy, it’s essential to continue to brush and floss. By maintaining proper oral hygiene, you’re preventing further problems as well as supporting healing and optimal oral health.
-
Get the tooth restored in a timely fashion
To rebuild the strength and integrity of a tooth that has received a root canal therapy, it needs to be restored with a permanent crown or suitable restoration. Until that time, the remaining tooth structure is weak and vulnerable to fracture. The sooner a permanent restoration is placed, the sooner you can bite and chew with confidence and ease.
With proper maintenance and care, a tooth that has been treated with root canal treatment can last a lifetime.
At the office of Hawthorn Dental Associates, we’re dedicated to providing the highest quality of care. If you have any additional concerns, continuing discomfort, or signs of an infection, or concerns following your procedure, contact our office for prompt attention and care.
FAQs
+Why have a root canal procedure?
A root canal procedure is the best way to save a tooth that has been damaged by decay or injury and preserve your natural smile. The alternative is an extraction and treatment to replace the tooth. While at times a tooth is non-restorable and an extraction is the only option, when possible, it’s best to try and save your natural tooth. With proper care, a tooth with root canal therapy care can serve your smile well for many years to come.
+Is a root canal procedure painful?
Despite lingering myths from before the age of modern dental anesthesia and technology, having a root canal procedure today is as routine and comfortable as visiting the dentist for a filling. While the procedure is performed under local anesthesia with your tooth completely numbed, we can also discuss options in dental sedation.
+Do I need to have a root canal procedure if I’m not in pain?
Whether the symptoms of a dental infection subside after a course of antibiotics, a draining abscess provides you with some temporary pain relief, or a tooth with radiographic evidence of pathology has not yet developed symptoms, it’s essential, before an infection worsens or occurs, to have a root canal procedure performed. In this way, the tooth can be disinfected, filled, and sealed to protect your health and avoid further problems.
+Do you offer emergency appointments?
If you have sustained a dental injury, have a toothache, jaw pain, swelling, or are experiencing any other unusual and uncomfortable oral symptoms, contact our office immediately for care. Dental problems that have not been evaluated and treated can significantly worsen, producing more severe damage and consequences for the involved teeth, your oral health, and even your overall wellbeing. Once you get in touch with our office, our friendly and compassionate office team will get you in for care at your earliest convenience.
+How long does a root canal procedure take?
While some root canal procedures can be completed in one visit, others may involve 2 or 3 appointments. How long it takes depends on various factors, including active infection, the number of canals in the tooth, and the tooth’s location or anatomy.
+How successful is root canal therapy?
With a success rate that exceeds 95%, root canal therapy remains the most effective procedure to save a tooth in which the inner vital tissues have been damaged. However, as with all healthcare procedures, there are a small percentage of cases where the teeth become symptomatic a second time. The good news is that many of these teeth can still be saved with root canal retreatment or a minor surgical procedure known as an apicoectomy.
+What’s the best way to take care of my tooth root canal therapy?
The best ways to maintain a tooth with root canal therapy are to get the proper restoration required to rebuild and protect the tooth, maintain proper oral hygiene, and schedule appointments for routine dental checkups and care.
+How much does root canal therapy cost, and does dental insurance cover it?
Saving a tooth with root canal therapy is a wise investment that, in the long run, is typically less costly and invasive than having the tooth extracted and replaced with a fixed bridge or implant. As far as the exact cost of care, it can vary depending on which tooth is being treated. Many dental insurance plans provide coverage for root canal therapy. At the office of Hawthorn Dental Associates, we do our best to optimize your dental benefits and minimize your out-of-pocket expenses. Our staff answer all your questions about the cost of care and discuss all your payment options.
+Why choose the office of Hawthorn Dental Associates?
At the office of Hawthorn Dental Associates, we use the latest technology and most effective methods of care to provide precise and gentle care. Our reputation for excellence is based upon a consistent record of achieving successful treatment outcomes while providing prompt, stress-free, and convenient treatment for every type of dental need.
Teeth that have been stained or darkened by food, tobacco use, age, medications or injury can be lightened and brightened by means of a non-invasive process known as teeth whitening.
Teeth whitening or bleaching simply refers to any process that will make the teeth appear whiter. While there are many over the counter options for teeth whitening, the most effective and safest teeth whitening systems are the professional strength products available at the dentist’s office. A dental professional whitening system offers a higher concentration of whitening components and delivers them to the teeth in the most efficient manner to achieve optimal results.
At our office, we offer two exceptional options for tooth whitening. You can choose either our custom bleaching trays, or the Opalescence Go Trays. Both of these are top-of the-line systems that will help transform the beauty and whiteness of your smile.
According to the National Institute of Dental and Craniofacial Research (NIDCR), temporomandibular joint disorders (TMJ), also referred to as temporomandibular disorders (TMD), are the most common source of chronic facial pain and jaw dysfunction. It is estimated that more than 10 million people in the United States are affected by temporomandibular joint problems.
What is the Temporomandibular Joint?
There are two temporomandibular joints that connect the left and right sides of the lower jaw to the temporal bone. Both joints and their associated muscles, ligaments and tendons work together to allow for all manner of oral function as the jaw moves up and down, front to back and from side to side. Containing a shock-absorbing, soft disc that sits between the rounded condyles of both sides of the lower jaw and the corresponding concavities in the skull’s temporal bone, the TMJ makes chewing, speaking, yawning and all jaw movements possible.
Since the TMJ is a joint with both up and down hinge-like movements, as well as side to side and front to back sliding motions to perform, it is often considered one of the most complicated joints in the body and one of the most difficult to treat when problems arise.
Types and Symptoms of TMJ Disorders
TMJ disorders can fall into one or more of the following three categories:
-
Myofascial pain- Refers to pain in the area of the jaw joint due to various causes of increased muscle tension and spasm
-
Internal derangement-Involves displacement of the disc, jaw dislocation or trauma to the condyles of the jaw
-
Degenerative joint disease -Arthritis
The risk for developing a TMJ problem is greater in the presence of long-term teeth grinding or bruxism, a jaw injury or various types of arthritis such as rheumatoid arthritis and osteoarthritis. Furthermore, the manifestations of a TMJ disorder can vary from person to person with a wide range of symptoms possible, including earaches, ringing in the ears (tinnitus), headaches, back and neck pain, vertigo, muscle spasms and joint tenderness as well as jaw pain, popping or grating sounds with jaw movement, jaw locking and limited jaw movement. For some people a TMJ disorder can be resolved within a relatively short period of time, while for others it will continue to persist despite extensive therapy.

Diagnosis and Treatment
When evaluating for the presence of a TMJ disorder, the dentist will perform a thorough clinical assessment of joint symptoms and function. Special radiographic imaging and other diagnostic tests will be ordered as needed. The treatment of a TMJ disorder may include oral appliances such as night guards or stabilization splints to alleviate strain on the joints. Other types of therapy may include steroid injections, occlusal adjustments as well as orthodontic or prosthodontic treatment to improve occlusion. In cases of persistent and serious TMJ problems, surgery may be recommended.
Methods of self-care can be helpful in alleviating some of the symptoms of a TMJ disorder. Patients are typically advised to eat soft foods, avoid extreme jaw movement such as wide yawning and gum chewing, to practice stress reduction and relaxation techniques and applying ice packs or moist heat as directed. If recommended, a patient should follow the dentist or therapist’s instruction for gentle stretching exercises. The short-term use of over-the-counter, non-steroidal, anti-inflammatory drugs and pain medications may provide relief. If not the dentist or physician may prescribe stronger pain or anti-inflammatory drugs, muscle relaxants or anti-depressants.
As the most recognizable expression and the universal sign of happiness, a beautiful smile is an important asset. Studies show that an attractive smile can boost your self-confidence, contribute to your overall well-being, and help make a positive impression on everyone you meet.
Transforming Smiles With Porcelain Veneers
If your front teeth are stained, discolored, chipped, worn-down, misshapen, a little gapped, or slightly misaligned, you're not alone. According to statistics, more than one-third of adults in the United States are dissatisfied with the appearance of their smiles. Cosmetic imperfections may be due to genetics, excessive wear and tear on the teeth, the aging process, dietary choices that stain the dental enamel, smoking, or as a side effect of certain medications.
In some cases, if the imperfections are minor ones, a teeth whitening procedure or cosmetic bonding may be all it takes to create a more perfect-looking smile. However, darker dental stains, discolorations, and more significant flaws involving the size, shape, and alignment of the teeth, are sometimes better addressed with porcelain veneers.
At the office of Hawthorn Dental Associates, we recognize that every smile is different and tailor treatment to address individual needs and expectations of care. Whether your smile is best served by the fabrication of dental veneers or another cosmetic dental procedure we provide, you can count on our office for the latest, most effective, pleasing, and healthy solutions for your smile.
What are dental veneers?
One of the most conservative yet highly effective and aesthetically pleasing ways to transform the appearance of imperfect looking teeth is the fabrication of dental veneers. Fully customized to the exact specifications of your smile and the cosmetic corrections required, veneers are ultra-thin facings, seamlessly bonded to the fronts of the involved teeth.
This versatile and minimally-invasive cosmetic procedure conceals a range of imperfections to dramatically improve the look of teeth that are misshapen, exhibit minor chips, enamel defects, or stains. They also provide an excellent solution for closing small gaps as well as addressing other minor alignment issues.
Among the chief benefits offered by veneers are that they require little to no preparation of the underlying tooth and offer a relatively quick way to achieve long-lasting and pleasing results. And because they are ultra-thin, veneers preserve the maximum amount of natural tooth structure and are kind to the tissues along the gumline.
With veneers, your smile looks naturally beautiful.
Whether you're looking to improve the appearance of a single front tooth or multiple ones, dental veneers can turn a less-than-perfect smile into one that appears naturally beautiful and flawless.
Your veneers are fabricated from the highest quality of dental-grade porcelain to recreate the natural translucency of healthy tooth enamel. Since porcelain reflects light in much the same way as dental enamel, veneers produce a vibrant, flawless, and naturally beautiful-looking smile.
From preparation to taking an impression and placement, the entire process of getting dental veneers only takes a few visits. Furthermore, even though a veneer is fragile to handle before placement in the mouth, once it gets bonded to the underlying tooth, it becomes quite strong and durable. With proper oral hygiene and care, you can maintain your new veneers for many years to come.
At the office of Hawthorn Dental Associates, we successfully combine the art and science of dentistry to create healthy, beautiful smiles. We've helped many patients enhance the look of their smiles and feel confident we can do the same for you.
What to expect when getting veneers
-
Initial consultation and care
The process of getting dental veneers begins with a consultation and thorough assessment of your dental health, oral function, and smile aesthetics. We'll also discuss your smile goals and treatment expectations. Although getting veneers is a relatively quick process, it's essential to address any periodontal problems or cavities in the involved teeth before your new veneers get fabricated.
-
Tooth preparation and Impression taking
While the amount of tooth preparation varies, depending on the unique requirements of the case and the type of porcelain veneer, the removal of tooth structure from the front and sides of the tooth is typically quite minimal. It's just enough enamel for the ultra-thin facing to look most natural and remain sturdy and strong when placed.
Once the teeth are prepared, an impression gets taken, and an appropriate shade of porcelain is selected, your new veneers are ready for fabrication. Porcelain veneers are most often sent out to a dental laboratory for custom fabrication. For the short time it takes the permanent ones to come back from the lab, attractive temporary veneer facings cover the teeth.
-
Fitting and placement
When your veneers are ready, it's time to check their fit, size, shade, and shape. Prior to getting affixed to the teeth, any adjustments to ensure a precise fit and optimal aesthetics are made. At this time, we'll also confirm that you're pleased with the look of your new smile. Once fitted and approved, the involved teeth are then cleaned, and the veneers are permanently bonded in place with composite resin cement. Following placement, any further adjustments or minor refinements are performed as needed.
Veneers FAQs
+Will I need a veneer or a crown?
Determining if a veneer is suitable or a full-coverage crown is required depends on the extent of the tooth's defects and the remaining amount of healthy tooth structure. For teeth with imperfections that cannot be remedied with a teeth whitening procedure, dental veneers often provide the desired cosmetic improvements. However, a significantly undersized, misshapen, chipped, or darkly stained tooth usually requires a full coverage crown.
+Do veneers look natural?
Porcelain veneers are fabricated from the highest grade of dental ceramics, which reflect light in much the same way as the enamel of natural teeth. In addition to this feature, dental porcelain is resistant to stains and discolorations, keeping your smile white and vibrant for years to come.
+How long do dental veneers last?
Porcelain veneers are ultra-thin customized facings that become strong and durable once bonded to the underlying teeth. With proper hygiene and routine dental care, veneers provide a cosmetic solution that not only looks and feels completely natural but is also long lasting.
However, just as harmful oral habits can affect your natural teeth, they can also cause damage to your veneers. To prevent chipping, cracking, or dislodging a veneer, avoid nail biting, chewing on hard candies, ice, pens, or pencils, and opening bottles or other objects with your teeth. Also, remember to protect your smile on the playing field by wearing a properly fitted sports mouthguard.
Tooth grinding or bruxism is another important consideration in care. If you clench or grind your teeth, you may need to wear a night guard to help protect your new smile or discuss other options with our office.
+How many veneers will I need?
As versatile as they are beautiful, dental veneers can be applied to a single tooth in need of cosmetic improvement or multiple front teeth to dramatically improve the look of your smile. Whatever the case may be, dental veneers provide highly satisfying results to create a smile; you'll feel confident sharing with the world.
+Can veneers address more than one cosmetic problem?
Among the many benefits offered by dental veneers is their ability to mask a range of imperfections at once. In addition to covering stains or discolorations on the front surface of a tooth, the size and shape of a veneer can also be customize to improve the tooth's contours and dimensions. At the same time veneers create a whiter and more vibrant smile; they can also lengthen or widen a tooth, close minor gaps, and address other minor alignment issues.
+Are there different types of veneers?
The two most common types of veneers are porcelain veneers, also known as porcelain laminates, and composite veneers. Although porcelain veneers are the most commonly offered option in care, composite veneers fabricated directly on the tooth can also achieve excellent results. You may have also heard the term no-prep veneer. It refers to a type of porcelain veneer that requires little to no preparation of the underlying dental enamel. At your consultation visit, we'll discuss your best options in care.
+With dental veneers, can I clean my teeth as before?
Once they're in place, your veneers are also easy to care for and maintain. Simply by brushing, flossing, and visiting our office for periodic checkups, you can successfully protect and preserve your new and beautiful smile.
+How much do dental veneers cost?
Although certain procedures that are considered cosmetic may not be covered by dental insurance, veneers remain a worthwhile investment in your smile. Based on the unique considerations of each case, we develop treatment plans that consider specific dental needs, cosmetic goals, and budget. Our experienced and friendly office staff can address all your insurance questions and review various payment and financing options.
+Why choose the office of Hawthorn Dental Associates?
At the office of Hawthorn Dental Associates, we value patient input and pay close attention to your treatment goals, concerns, and expectations in care. When it comes to cosmetic dentistry, we recognize that every smile is unique and never take a “one size fits all” approach to care. We utilize the most advanced diagnostic technology and treatment methods to assess your smile and to design your porcelain veneers for a precise fit and optimal aesthetics.
As experienced providers of care, we provide highly personalized treatment, combining state-of-the-art technology with an artistic touch to produce long-lasting and aesthetically pleasing results of care.
